UNITED STATES
SECURITIES AND EXCHANGE COMMISSION
WASHINGTON, D.C. 20549
FORM 8-K
CURRENT REPORT
Pursuant to Section 13 or 15(d) of the Securities Exchange Act of 1934
Date of Report (Date of earliest event reported): March 24, 2025 |
Aura Biosciences, Inc.
(Exact name of Registrant as Specified in Its Charter)
Delaware |
001-40971 |
32-0271970 |
||
(State or Other Jurisdiction |
(Commission File Number) |
(IRS Employer |
||
|
|
|
|
|
80 Guest Street |
|
|||
Boston, Massachusetts |
|
02135 |
||
(Address of Principal Executive Offices) |
|
(Zip Code) |
||
Registrant’s Telephone Number, Including Area Code: 617 500-8864 |
Not Applicable |
(Former Name or Former Address, if Changed Since Last Report)
Check the appropriate box below if the Form 8-K filing is intended to simultaneously satisfy the filing obligation of the registrant under any of the following provisions:
Securities registered pursuant to Section 12(b) of the Act:
|
|
Trading |
|
|
Common Stock, $0.00001 par value per share |
|
AURA |
|
The Nasdaq Global Market |
Indicate by check mark whether the registrant is an emerging growth company as defined in Rule 405 of the Securities Act of 1933 (§ 230.405 of this chapter) or Rule 12b-2 of the Securities Exchange Act of 1934 (§ 240.12b-2 of this chapter).
Emerging growth company ☒
If an emerging growth company, indicate by check mark if the registrant has elected not to use the extended transition period for complying with any new or revised financial accounting standards provided pursuant to Section 13(a) of the Exchange Act. ☐
Item 2.02 Results of Operations and Financial Condition.
On March 24, 2025, Aura Biosciences, Inc. (the “Company”) issued a press release announcing its financial results for the fourth quarter and year ended December 31, 2024. A copy of the press release is furnished as Exhibit 99.1 to this Current Report on Form 8-K.
The information in this Item 2.02, including Exhibit 99.1 hereto, shall not be deemed “filed” for purposes of Section 18 of the Securities Exchange Act of 1934, as amended (the “Exchange Act”), or otherwise subject to the liabilities of that section, nor shall it be deemed incorporated by reference in any filing under the Securities Act of 1933, as amended, or the Exchange Act, except as expressly set forth by specific reference in such a filing.
Item 8.01 Other Events.
On March 24, 2025, the Company updated its corporate presentation for use in meetings with investors, analysts, and others. A copy of the corporate presentation is filed as Exhibit 99.2 for purposes of Section 18 of the Exchange Act.
Forward Looking Statements
Statements contained under this Item 8.01 regarding matters that are not historical facts are “forward-looking statements” within the meaning of the Private Securities Litigation Reform Act of 1995. Because such statements are subject to risks and uncertainties, actual results may differ materially from those expressed or implied by such forward-looking statements. Such statements include, but are not limited to, statements about the initiation, timing, progress, results, and cost of the Company’s research and development programs and the Company’s current and future preclinical studies and clinical trials, including statements regarding the timing of initiation and completion of studies or trials and related preparatory work, the period during which the results of the trials will become available, and the Company’s research and development programs; statements regarding the Company’s expectations for an improved quality of life of patients after treatment with bel-sar and changes to the treatment paradigm for patients; the Company’s ability to successfully manufacture its drug substances and product candidates for preclinical use, for clinical trials and on a larger scale for commercial use, if approved; the ability and willingness of the Company’s third-party strategic collaborators to continue research and development activities relating to the Company’s development candidates and product candidates; the Company’s ability to commercialize its products, if approved; the Company’s ability to obtain funding for its operations necessary to complete further development and commercialization of its product candidates; the Company’s ability to obtain and maintain regulatory approval of its product candidates; statements regarding the Company’s beliefs and expectations for the high unmet medical need for an effective local treatment in ocular and urologic oncology to preserve organ function; the size and growth potential of the markets for the Company’s product candidates, and the Company’s ability to serve those markets; the Company’s financial performance; the Company’s expected cash runway into the second half of 2026; and the implementation of the Company’s business model, including strategic plans for its business and product candidates.
Any forward-looking statements are neither promises nor guarantees, and investors should not place undue reliance on these forward-looking statements because they involve known and unknown risks, uncertainties, and other factors, many of which are beyond the Company’s control and which could cause actual results to differ materially from those expressed or implied by these forward-looking statements, including, without limitation, uncertainties inherent in clinical trials and in the availability and timing of data from ongoing clinical trials; the expected timing for submissions for regulatory approval or review by governmental authorities; the risk that the results of the Company’s preclinical and clinical trials may not be predictive of future results in connection with future clinical trials; the risk that interim data from ongoing clinical trials may not be predictive of final data from completed clinical trials; the risk that governmental authorities may disagree with the Company’s clinical trial designs even where the Company has obtained agreement with governmental authorities on the design of such trials, such as the Phase 3 Special Protocol agreement with the United States Food and Drug Administration; whether the Company will receive regulatory approvals to conduct trials or to market products; whether the Company’s cash resources will be sufficient to fund its foreseeable and unforeseeable operating expenses and capital expenditure requirements; the Company’s ongoing and planned preclinical activities; and the Company’s ability to initiate, enroll, conduct or complete ongoing and planned clinical trials. These risks, uncertainties, and other factors include those risks and uncertainties described under the heading “Risk Factors” in the Company’s most recent Annual Report on Form 10-K and Quarterly Report on Form 10-Q filed with the United States Securities and Exchange Commission (“SEC”) and in subsequent filings made by the Company with the SEC, which are available on the SEC’s website at www.sec.gov. Except as required by law, the Company disclaims any intention or responsibility for updating or revising any forward-looking statements contained under this Item 8.01 in the event of new information, future developments or otherwise. These forward-looking statements are based on the Company’s current expectations and speak only as of the date hereof and no representations or warranties (express or implied) are made about the accuracy of any such forward-looking statements.
Item 9.01 Financial Statements and Exhibits.
(d) Exhibits.
Exhibit No. |
Description |
99.1 |
|
99.2 |
|
104 |
Cover Page Interactive Data File (embedded within the Inline XBRL document). |
SIGNATURES
Pursuant to the requirements of the Securities Exchange Act of 1934, the registrant has duly caused this report to be signed on its behalf by the undersigned hereunto duly authorized.
|
|
|
Aura Biosciences, Inc. |
|
|
|
|
Date: |
March 24, 2025 |
By: |
/s/ Amy Elazzouzi |
|
|
|
Amy Elazzouzi (Interim Principal Financial Officer and Interim Principal Accounting Officer) |
Exhibit 99.1

Aura Biosciences Reports Fourth Quarter and Full Year 2024 Financial Results and Business Highlights
Positive Phase 1 Trial Data in Non-Muscle Invasive Bladder Cancer (NMIBC) Presented at the 40th Annual European Association of Urology Congress; Supports Front-Line Treatment Potential
Clinical Pipeline Continues to Advance with Phase 3 CoMpass Trial Actively Enrolling
Phase 2 Trial in Metastases to the Choroid Initiated
Cash Position Expected to Support Operations into 2H 2026
BOSTON, MA – March 24, 2025 – Aura Biosciences, Inc. (NASDAQ: AURA), a clinical-stage biotechnology company developing precision therapies for solid tumors designed to preserve organ function, today reported financial results for the fourth quarter and year ended December 31, 2024, and provided recent business highlights.
“We believe that bel-sar has the potential to transform the treatment paradigm in multiple rare oncology indications starting with ocular cancers and more broadly across many solid tumors such as bladder cancer. The data presented from the Phase 2 trial in early-stage choroidal melanoma and the Phase 1 trial in NMIBC demonstrated bel-sar’s potential as a front-line treatment option across multiple tumor types,” said Elisabet de los Pinos, Chief Executive Officer of Aura Biosciences. “These data highlight the potential clinical benefit of a novel dual mechanism of action driven by highly targeted cytotoxicity and robust cell-mediated immunity. We look forward to continuing to advance our pipeline across multiple indications with high unmet patient need.”
Recent Pipeline Developments
Early-Stage Choroidal Melanoma
Early-stage choroidal melanoma represents an area of high unmet need with no drugs approved. The Company previously received Orphan Drug Designation from the United States Food and Drug Administration (FDA) and the European Medicines Agency (EMA) and Fast Track designation from the FDA for the treatment of early-stage choroidal melanoma. The CoMpass trial is under a Special Protocol Assessment (SPA) agreement with the FDA.
Update on Ongoing Phase 3 CoMpass Trial: CoMpass is the first registration-enabling study in early-stage choroidal melanoma. The study is a global, Phase 3, randomized trial evaluating bel-sar treatment against a sham control arm and includes an enrichment strategy to enroll approximately 100 patients with documented tumor growth.
|
|
|
The CoMpass trial is actively enrolling globally. To identify appropriate patients to meet the enrichment strategy of documented growth, the Company has enabled a pre-screening ‘run in’ period. Globally, since June 2024, investigators have registered over 175 patients in pre-screening as having met initial enrollment criteria for the study. The acceleration in pre-screening is driven by increasing momentum in the United States and European Union.
Additional Ocular Oncology Indications:
In addition to early-stage choroidal melanoma, bel-sar is being explored for metastases to the choroid and cancers of the ocular surface. These three ocular oncology indications have a collective incidence of greater than 60,000 patients annually in the United States and Europe.
Metastases to the Choroid
The Company has initiated a Phase 2 clinical trial in metastases to the choroid and has sites activated with patients in prescreening. Metastases to the choroid is an indication with high unmet medical need and no approved therapies. The Company expects initial data from this trial in 2025.
Metastases to the choroid represents the second potential ocular oncology indication for bel-sar, affecting approximately 20,000 patients annually in the United States and Europe. The Company previously received FDA Fast Track designation for bel-sar in this indication.
Cancers of the Ocular Surface
The Company’s third potential ocular oncology indication is cancers of the ocular surface, which affects approximately 35,000 patients in the United States and Europe annually. The Company continues to advance its preclinical work designed to be IND-enabling in cancers of the ocular surface.
Bladder Cancer
Positive additional data from the Company’s Phase 1 trial of bel-sar in patients with NMIBC was presented at the 40th Annual European Association of Urology Congress. In totality, the data demonstrate clinical complete responses as well as robust cell mediated immunity across the intermediate- and high-risk disease spectrum.
These data now include the histopathological assessment of all 10 patients after treatment with light activation and the full evaluation of safety and tumor response in two additional patients with high-risk NMIBC. One patient with high-risk disease (due to BCG failure) demonstrated a clinical complete response. Further, to evaluate the local immune response after the treatment with bel-sar in the TME, multiplex immunofluorescence staining for key immune cell types was performed on tumor biopsies from three patients. These early observations show induction of effector immunity and the development of local active immunosurveillance, highlighting key features of bel-sar’s dual mechanism of action and the potential to translate into durable treatment responses. The Company previously announced early data from this Phase 1 trial in October 2024. Details of the updated results of the Phase 1 NMIBC trial can be found here.
|
|
|
Corporate Updates
Full Year and Fourth Quarter 2024 Financial Results
|
|
|
About Aura Biosciences
Aura Biosciences is a clinical-stage biotechnology company focused on developing precision therapies for solid tumors that aim to preserve organ function. Our lead candidate, bel-sar (AU-011), is currently in late-stage development for primary choroidal melanoma and in early-stage development in other ocular oncology indications and bladder cancer. Aura Biosciences is headquartered in Boston, MA. Our mission is to grow as an innovative global oncology company that positively transforms the lives of patients.
For more information, visit aurabiosciences.com. Follow us on X (formerly Twitter) @AuraBiosciences and visit us on LinkedIn.
Forward-Looking Statements
This press release contains forward-looking statements within the meaning of the Private Securities Litigation Reform Act of 1995, as amended, and other federal securities laws. Any statements that are not statements of historical fact may be deemed to be forward-looking statements. Words such as “may,” “will,” “could,” “should,” “expects,” “intends,” “plans,” “anticipates,” “believes,” “estimates,” “predicts,” “projects,” “seeks,” “endeavor,” “potential,” “continue” or the negative of such words or other similar expressions can be used to identify forward-looking statements. These forward-looking statements include express or implied statements regarding Aura’s future expectations, plans and prospects, including, without limitation, statements regarding the therapeutic potential of bel-sar for the treatment of multiple cancers; statements regarding Aura’s plans and expectations for its ongoing and future clinical trials of bel-sar in multiple oncology indications; statements regarding the timing and plans to present initial data with respect to its Phase 2 clinical trial of bel-sar for the treatment of metastases to the choroid; statements regarding Aura’s expectations for an improved quality of life of patients after treatment with bel-sar and changes to the treatment paradigm for patients; statements regarding Aura’s expectations for the estimated patient populations and related market opportunities for bel-sar; and statements regarding the Company’s expected cash runway.
|
|
|
The forward-looking statements in this press release are neither promises nor guarantees, and investors should not place undue reliance on these forward-looking statements because they involve known and unknown risks, uncertainties and other factors, many of which are beyond Aura’s control and which could cause actual results to differ materially from those expressed or implied by these forward-looking statements, including, without limitation, uncertainties inherent in clinical trials and in the availability and timing of data from ongoing clinical trials; the expected timing for submissions for regulatory approval or review by governmental authorities; the risk that the results of Aura’s preclinical and clinical trials may not be predictive of future results in connection with future clinical trials; the risk that early or interim data from ongoing clinical trials may not be predictive of final data from completed clinical trials; the risk that governmental authorities may disagree with Aura’s clinical trial designs, even where Aura has obtained agreement with governmental authorities on the design of such trials, such as the Phase 3 special protocol assessment agreement with the U.S. Food and Drug Administration; whether Aura will receive regulatory approvals to conduct trials or to market products; whether Aura’s cash resources will be sufficient to fund its foreseeable and unforeseeable operating expenses and capital expenditure requirements; Aura’s ongoing and planned preclinical activities; and Aura’s ability to initiate, enroll, conduct or complete ongoing and planned clinical trials. These risks, uncertainties and other factors include those risks and uncertainties described under the heading “Risk Factors” in Aura’s most recent Annual Report on Form 10-K and Quarterly Report on Form 10-Q filed with the United States Securities and Exchange Commission (SEC) and in subsequent filings made by Aura with the SEC, which are available on the SEC’s website at www.sec.gov. Except as required by law, Aura disclaims any intention or responsibility for updating or revising any forward-looking statements contained in this press release in the event of new information, future developments or otherwise. These forward-looking statements are based on Aura’s current expectations and speak only as of the date hereof and no representations or warranties (express or implied) are made about the accuracy of any such forward-looking statements.
Investor and Media Relations Contact:
Alex Dasalla
Head of Investor Relations and Corporate Communications
IR@aurabiosciences.com
|
|
|
Aura Biosciences, Inc.
Consolidated Statement of Operations and Comprehensive Loss
(in thousands, except share and per share amounts)
|
|
Year Ended |
|
|||||
|
|
2024 |
|
|
2023 |
|
||
Operating Expenses: |
|
|
|
|
|
|
||
Research and development |
|
$ |
73,302 |
|
|
$ |
65,232 |
|
General and administrative |
|
|
22,814 |
|
|
|
19,759 |
|
Total operating expenses |
|
|
96,116 |
|
|
|
84,991 |
|
Total operating loss |
|
|
(96,116 |
) |
|
|
(84,991 |
) |
Other income (expense): |
|
|
|
|
|
|
||
Interest income, including amortization and accretion income |
|
|
9,429 |
|
|
|
8,588 |
|
Gain on disposal of property and equipment |
|
|
— |
|
|
|
208 |
|
Other expense |
|
|
(120 |
) |
|
|
(76 |
) |
Total other income |
|
|
9,309 |
|
|
|
8,720 |
|
Loss before income taxes |
|
|
(86,807 |
) |
|
|
(76,271 |
) |
Income tax provision, net |
|
|
(112 |
) |
|
|
(137 |
) |
Net loss |
|
|
(86,919 |
) |
|
|
(76,408 |
) |
Net loss per common share—basic and diluted |
|
|
(1.75 |
) |
|
|
(1.93 |
) |
Weighted average common stock outstanding—basic and diluted |
|
|
49,650,480 |
|
|
|
39,620,036 |
|
Comprehensive loss: |
|
|
|
|
|
|
||
Net loss |
|
$ |
(86,919 |
) |
|
$ |
(76,408 |
) |
Other comprehensive items: |
|
|
|
|
|
|
||
Unrealized (loss) gain on marketable securities |
|
|
(271 |
) |
|
|
611 |
|
Other |
|
|
(5 |
) |
|
|
— |
|
Total other comprehensive (loss) income |
|
|
(276 |
) |
|
|
611 |
|
Total comprehensive loss |
|
$ |
(87,195 |
) |
|
$ |
(75,797 |
) |
|
|
|
Aura Biosciences, Inc.
Consolidated Balance Sheets
(in thousands, except share and per share amounts)
|
|
December 31, 2024 |
|
|
December 31, 2023 |
|
||
Assets |
|
|
|
|
|
|
||
Current assets: |
|
|
|
|
|
|
||
Cash and cash equivalents |
|
$ |
31,693 |
|
|
$ |
41,063 |
|
Marketable securities |
|
|
119,401 |
|
|
|
185,087 |
|
Restricted cash and deposits |
|
|
— |
|
|
|
19 |
|
Prepaid expenses and other current assets |
|
|
9,529 |
|
|
|
5,625 |
|
Total current assets |
|
|
160,623 |
|
|
|
231,794 |
|
Restricted cash and deposits, net of current portion |
|
|
768 |
|
|
|
768 |
|
Right-of-use assets - operating lease |
|
|
17,379 |
|
|
|
18,854 |
|
Other long-term assets |
|
|
518 |
|
|
|
509 |
|
Property and equipment, net |
|
|
3,215 |
|
|
|
3,150 |
|
Total Assets |
|
$ |
182,503 |
|
|
$ |
255,075 |
|
Liabilities and Stockholders’ Equity |
|
|
|
|
|
|
||
Current liabilities: |
|
|
|
|
|
|
||
Accounts payable |
|
|
2,304 |
|
|
|
1,787 |
|
Short-term operating lease liability |
|
|
3,149 |
|
|
|
2,687 |
|
Accrued expenses and other current liabilities |
|
|
9,460 |
|
|
|
7,883 |
|
Total current liabilities |
|
|
14,913 |
|
|
|
12,357 |
|
Long-term operating lease liability |
|
|
15,620 |
|
|
|
16,870 |
|
Total Liabilities |
|
|
30,533 |
|
|
|
29,227 |
|
Commitments and Contingencies |
|
|
|
|
|
|
||
Stockholders’ Equity: |
|
|
|
|
|
|
||
Common stock, $0.00001 par value, 150,000,000 authorized at December 31, 2024 and December 31, 2023, and 49,998,279 and 49,350,788 shares issued and outstanding at December 31, 2024 and December 31, 2023, respectively |
|
|
— |
|
|
|
— |
|
Additional paid-in capital |
|
|
525,934 |
|
|
|
512,617 |
|
Accumulated deficit |
|
|
(374,227 |
) |
|
|
(287,308 |
) |
Accumulated other comprehensive income |
|
|
263 |
|
|
|
539 |
|
Total Stockholders’ Equity |
|
|
151,970 |
|
|
|
225,848 |
|
Total Liabilities and Stockholders’ Equity |
|
$ |
182,503 |
|
|
$ |
255,075 |
|
|
|
|

Innovating the future of cancer care to cure patients and preserve organ function March 2025 Exhibit 99.2

Legal disclosure This presentation contains forward-looking statements, all of which are qualified in their entirety by this cautionary statement. Many of the forward-looking statements contained herein can be identified by the use of forward-looking words such as "may", "anticipate", "believe", "could', "expect", "should", "plan", "intend", "estimate", "will", "potential" and "ongoing", among others, although not all forward-looking statements contain these identifying words. These forward-looking statements include statements about the initiation, timing, progress, results and cost of our research and development programs and our current and future preclinical studies and clinical trials, including statements regarding the timing of initiation and completion of studies or trials and related preparatory work, the period during which the results of the trials will become available and our research and development programs; statements regarding our expectations for an improved quality of life of patients after treatment with bel-sar and changes to the treatment paradigm for patients; our ability to successfully manufacture our drug substances and product candidates for preclinical use, for clinical trials and on a larger scale for commercial use, if approved; the ability and willingness of our third-party strategic collaborators to continue research and development activities relating to our development candidates and product candidates; our ability to commercialize our products, if approved; our ability to obtain funding for our operations necessary to complete further development and commercialization of our product candidates; our ability to obtain and maintain regulatory approval of our product candidates; statements regarding our beliefs and expectations for the high unmet medical need for an effective local treatment in ocular and urologic oncology to preserve organ function; the size and growth potential of the markets for our product candidates and our ability to serve those markets; our financial performance; our expected cash runway into the second half of 2026; and the implementation of our business model, including strategic plans for our business and product candidates. Except as otherwise noted, these forward-looking statements speak only as of the date of this presentation, and we undertake no obligation to update or revise any of such statements to reflect events or circumstances occurring after this presentation. Because forward-looking statements are inherently subject to risks and uncertainties, some of which cannot be predicted or quantified and some of which are beyond our control, you should not rely on these forward-looking statements as predictions of future events. For a discussion of these and other risks and uncertainties, and other important factors, any of which could cause our actual results to differ from those contained in the forward-looking statements, see the section entitled "Risk Factors" in our most recent Annual Report on Form 10-K and Quarterly Report on Form 10-Q filed with the Securities and Exchange Commission (SEC), as well as discussions of potential risks, uncertainties, and other important factors in our other subsequent filings with the SEC, which are available on the SEC's website at www.sec.gov. The events and circumstances reflected in our forward-looking statements may not be achieved or occur and actual results could differ materially from those projected in the forward-looking statements. We caution you not to place undue reliance on the forward-looking statements contained in this presentation. This presentation discusses product candidates that are under preclinical or clinical evaluation and that have not yet been approved for marketing by the U.S. Food and Drug Administration (FDA) or any other regulatory authority. Until finalized in a clinical study report, clinical trial data presented herein remain subject to adjustment as a result of clinical site audits and other review processes. No representation is made as to the safety or effectiveness of these product candidates for the use for which such product candidates are being studied. This presentation shall not constitute an offer to sell or the solicitation of an offer to buy, nor shall there be any sale of these securities in any state or other jurisdiction in which such offer, solicitation or sale would be unlawful prior to registration or qualification under the securities laws of any such state or other jurisdiction.

1. Yu G-P et al. Am J Ophthalmol. 2003;135(6):800-6. 2. Triay E et al. Br J Ophthalmol. 2009;93(11):1524-8. 3. Newton R et al. Lancet. 1996;347(9013):1450-1. 4. Dalvin LA. Br J Ophthalmol. 2018;102(12):1728-1734. 5. Sun EC et al. Cancer Epidemiol Biomarkers Prev. 1997;6(2):73-7. 6. Epidemiology analysis for choroidal melanoma and choroidal metastasis by ClearView Healthcare Partners and Putman. 7. American Cancer Society. Key statistics for retinoblastoma. Available at: https://www.cancer.org/cancer/types/retinoblastoma/about/key-statistics.html. Accessed Sept 5, 2024. 8. Bladder cancer. Putnam & Assoc. Epidemiology Analysis.FDA, United States Food and Drug Administration; SPA, Special Protocol Assessment; VDC, Virus-like drug conjugate, MoA, Mechanism of action; NMIBC, Non-muscle-invasive bladder cancer Well positioned with multiple near-term clinical catalysts VDCs have the potential to transform early cancer treatment Novel MoA: direct tumor cell killing and immune cell activation Novel class of drugs virus-like drug conjugates Positive phase 2 data in early-stage choroidal melanoma with phase 3 ongoing under FDA SPA agreement Multiple clinical complete responses with single low dose in phase 1 trial in NMIBC Positive clinical data in multiple indications Ocular oncology >60,000 patients/yr (US/EU)1–7 Urologic oncology ~500,000 patients/yr (globally)8 Large market opportunity in areas of unmet need Multiple clinical datareadouts expected in 2025: initial data in phase 1b/2 in NMIBC and phase 2 in metastases to the choroid Cash expected to fundoperations into 2H 2026 Key upcoming catalysts
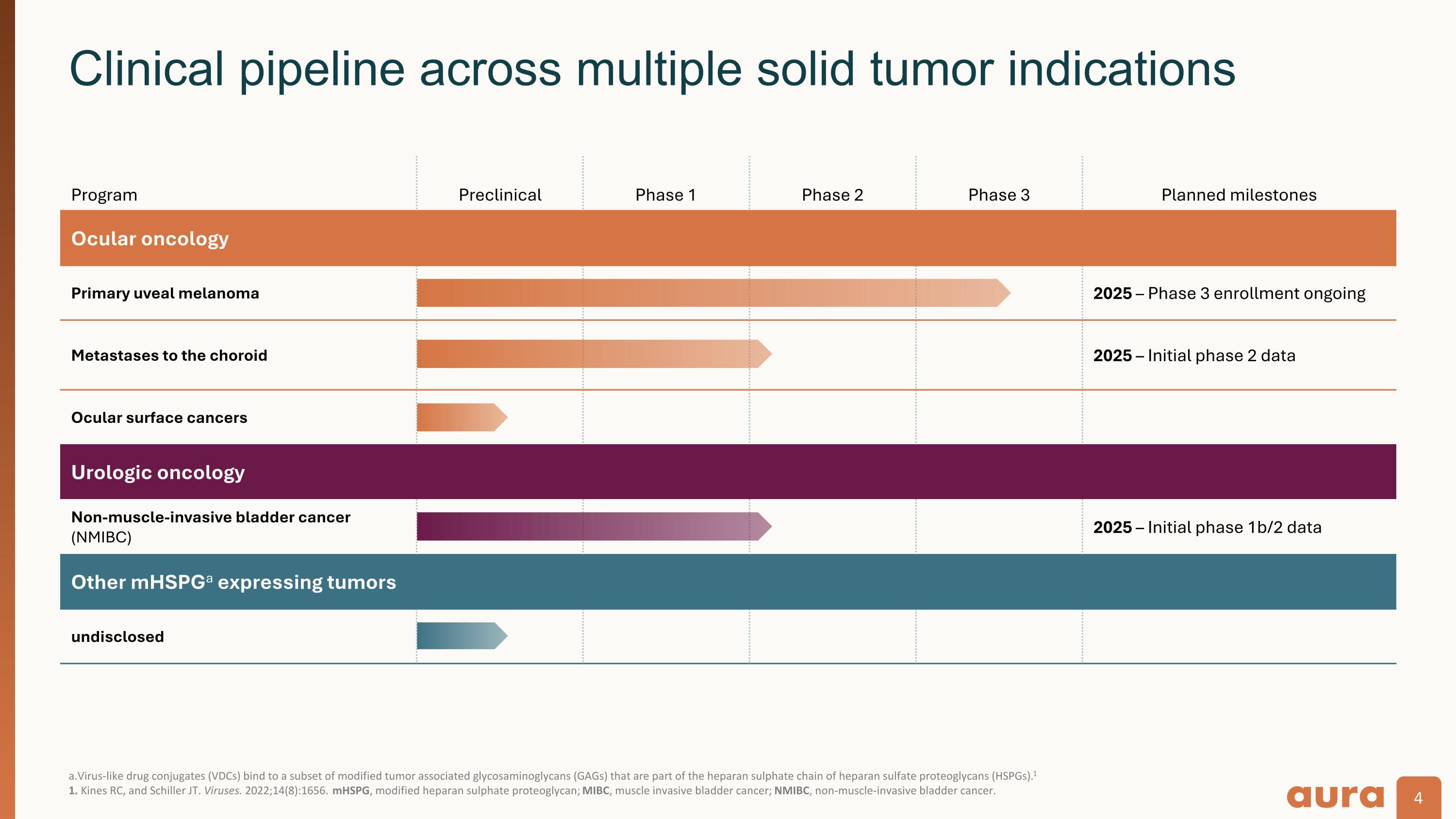
a.Virus-like drug conjugates (VDCs) bind to a subset of modified tumor associated glycosaminoglycans (GAGs) that are part of the heparan sulphate chain of heparan sulfate proteoglycans (HSPGs).11. Kines RC, and Schiller JT. Viruses. 2022;14(8):1656. mHSPG, modified heparan sulphate proteoglycan; MIBC, muscle invasive bladder cancer; NMIBC, non-muscle-invasive bladder cancer. Clinical pipeline across multiple solid tumor indications Program Preclinical Phase 1 Phase 2 Phase 3 Planned milestones Ocular oncology Primary uveal melanoma 2025 – Phase 3 enrollment ongoing Metastases to the choroid 2025 – Initial phase 2 data Ocular surface cancers Urologic oncology Non-muscle-invasive bladder cancer (NMIBC) 2025 – Initial phase 1b/2 data Other mHSPGa expressing tumors undisclosed

DLT, dose-limiting toxicity; MoA, mechanism of action; NMIBC, non-muscle-invasive bladder cancer; SAE, serious adverse event; VLP, virus-like particle. Virus-like drug conjugates have the potential to transform early cancer treatment 5 Positive clinical data in multiple early-stage local cancers Choroidal melanoma: Positive phase 2 end of study data; phase 3 ongoing NMIBC: Positive phase 1 data; phase 1b/2 trial initiated; enrollment expected to begin Q2 2025 Favorable safety profile Unique tumor selectivity Dual MoA Targets a key receptor molecule expressed in the early stages of malignant tumor transformation Targeted cytotoxicity and immune activation; potential to generate lasting anti-tumor T-cell memory Tumor and mutation-agnostic High potency >100 cell lines >15 animal tumor models ~200 cytotoxic molecules per VLP; demonstrated picomolar efficacy in multiple animal tumor models No treatment-related SAEs and no DLTs reported in phase 2 choroidal melanoma trial or phase 1 data readout in NMIBC trial

AU-011 has a novel dual mechanismof action Disruption of the tumorcell membrane andpro-immunogenic cell deathby necrosis leads to T cell activation and immune-mediated tumor cell killing Kines RC, et al. Int J Cancer. 2016;138(4):901–11. Kines RC, et al. Mol Cancer Ther. 2018;17(2):565–74. Kines RC, et al. Cancer Immunol Res. 2021;9:693–706.DAMPs, damage-associated molecular patterns; HSPG, heparan sulfate proteoglycan; VDC, virus-like drug conjugate; VLP, virus-like particle. Release of DAMPs induces anti-tumor immunity AU-011 treatment is designed to be cytopathic to resident suppressor cells, reducing the immune-suppressive microenvironment and contributing to anti-tumor immunity VLPs bind to macrophages, B cells, dendritic cells and neutrophils and are capable of stimulating antigen-presenting cells through TLR-4 engagement and NFk-β production Reactive oxygen species disrupts cell membrane and organelles

Bel-sar, belzupacap sarotalocan; CR, clinical complete response; CNS, central nervous system; GI, gastrointestinal; IND, Investigational New Drug application; MIBC, muscle-invasive bladder cancer; NMIBC, non-muscle-invasive bladder cancer; SPA, Special Protocol Assessment. Bel-sar’s unique platform technology is potentially applicable across multiple cancers Urologic oncology Other cancers Bladder cancer NMIBC/MIBC Positive phase 1 data in NMIBC Multiple CRs with single dose Phase 1b/2 trial initiated Potential to expand to MIBC Other urologic cancers Next-gen combination strategies CNS cancers GI cancers Head and neck cancer Breast cancer Lung cancer Cutaneous melanoma Ocular oncology - Rare oncology Choroidal melanoma Ongoing phase 3 with SPA Based on positive phase 2 clinical data Metastases to the choroid Phase 2 initiated Cancers of the ocular surface Pre-IND Retinoblastoma (pediatric) Pre-clinical

Ocular Oncology Bel-sar target indications: Primary uveal melanoma | Metastases to the choroid | Ocular surface cancers

Bel-sar opportunities in ocular oncology represent a multi-billion-dollar addressable market With only ~100 ocular oncologists in the US/EU,a global launch may be accomplished with a small(<20) field-based team aIncludes conjunctival melanoma, primary acquired melanosis, squamous cell carcinoma and ocular surface squamous neoplasia.1-5 1. Yu G-P et al. Am J Ophthalmol. 2003;135(6):800-6. 2. Triay E et al. Br J Ophthalmol. 2009;93(11):1524-8. 3. Newton R et al. Lancet. 1996;347(9013):1450-1. 4. Dalvin LA. Br J Ophthalmol. 2018;102(12):1728-1734. 5. Sun EC et al. Cancer Epidemiol Biomarkers Prev. 1997;6(2):73-7. 6. Epidemiology analysis for choroidal melanoma and choroidal metastasis by ClearView Healthcare Partners and Putman. 7. American Cancer Society. Key statistics for retinoblastoma. Available at: https://www.cancer.org/cancer/types/retinoblastoma/about/key-statistics.html. Accessed Sept 5, 2024. Bel-sar (AU-011) is an investigational product candidate. The effectiveness and safety of bel-sar have not been established, and bel-sar is not approved for use in any jurisdiction. Ocular surface cancers ~66,000 patients/year ~35,000/yra,1–5 Primary uveal melanoma ~11,000/yr6 Metastases to the choroid ~20,000/yr6 Retinoblastoma ~500/yr7 Ocular oncology franchise total addressable market (US/EU)

Bel-sar is in phase 3 for primary uveal melanoma, the most common primary intraocular cancerin adults Primary uveal melanoma is a high unmet medical need With no approved vision-preserving therapies, the current standard-of-care is radiotherapy – treatment that leads to legal blindness4,5 1. Heiting, G. Iris/uvea of the eye. Available at: https://www.allaboutvision.com/en-gb/resources/uvea-iris-choroid/. Accessed Oct. 3, 2023. 2. Kaliki S and Shields CL. Eye (Lond). 2017;31(2):241-257. 3. Epidemiology analysis for choroidal melanoma and choroidal metastasis by ClearView Healthcare Partners and Putman. 4. Jarczak J, Karska-Basta I, Romanowska-Dixon B. Deterioration of visual acuity after brachytherapy and proton therapy of uveal melanoma, and methods of counteracting this complication based on recent publications. Medicina (Kaunas). 2023;59(6):1131. 5.. Tsui I, Beardsley RM, McCannel TA, Oliver SC, et al. Visual acuity, contrast sensitivity and color vision three years after iodine-125 brachytherapy for choroidal and ciliary body melanoma. Open Ophthalmol J. 2015;9:131-5. Choroid is 90% of the uvea1 Uvea: Choroid, ciliary body and iris Ciliary body Iris Most common primary intraocular cancer in adults2,3 50% of patients develop metastasis within 15 years (metastatic uveal melanoma)2 ~80% of patients diagnosed with early-stage disease3 Choroidal melanoma ~11,000/yr3 Bel-sar has the potential to provide a treatment option that preserves vision

aEach figure represents ~250 persons. Shields CL et al. Choroidal and ciliary body melanoma. Available at: https://eyewiki.aao.org/Choroidal_and_Ciliary_Body_Melanoma Accessed September 9, 2024. Singh AD, et al. Ophthalmology. 2005;112(10):1784–89. Epidemiology analysis for choroidal melanoma and choroidal metastasis by ClearView Healthcare Partners and Putman. CM, choroidal melanoma; Enuc., enucleation. Current treatment paradigm for primary uveal melanoma Indeterminate lesions Small melanomas Risk Factors Growth Small CM Observation Incidence: Patients US/EUa Local – Early (~8,000) Local – Late (~2,300) Metastatic (~2,000) SIZE (mm): Small Medium Large Metastatic Radiotherapy Radiotherapy 1 2.5 – 3 >10 Enuc. Systemic chemotherapy (KIMMTRAK®)

1. Jarczak J et al. Medicina (Kaunas). 2023;59(6):1131. 2. Tsui I, et al. Open Ophthalmol J. 2015;9:131–5. 3. Shields CL, et al. Arch Ophthalmol. 2000;118(9):1219–1228. 4. Peddada KV, et al. J Contemp Brachytherapy. 2019;11(4):392–397.5. Shields CL et al. Curr Opin Ophthalmol. 2019;30(3):206–214. 6. Kaliki S, Shields CL. Eye. 2017;31(2):241–257. AE, adverse event; BCVA, best-corrected visual acuity; HRVL, high-risk for vision loss. High morbidity associated with current standard of care Up to 87% of primary uveal melanoma patients become legally blind over time in the eye treated with radiotherapy1,2 Radiotherapy3–6 Adverse Event Surgeries secondary to AEs (e.g., cataracts) 40%+ Radiation retinopathy 40%+ Neovascular glaucoma 10% Dry eye syndrome 20% Strabismus 2%+ Retinal detachment 1–2% Vision loss (≥15 letters) ~70% Long-term legal blindness (≤20/200) ~90% Serious Adverse Event Scleral necrosis 0–5% Enucleation/eye loss 10–15% Severe vision loss (≥30 letters) in HRVL ~90%
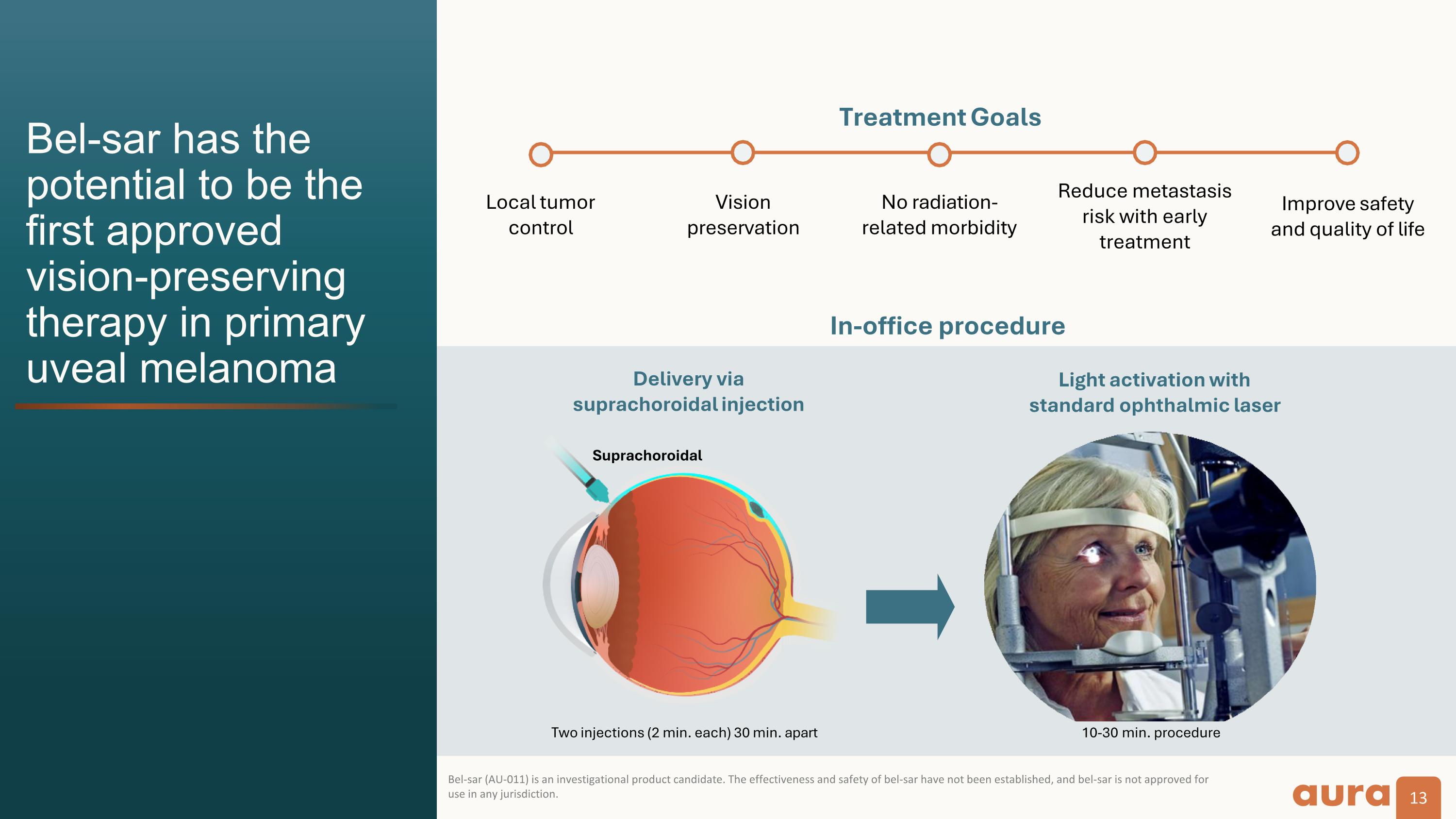
Bel-sar has the potential to be the first approved vision-preserving therapy in primary uveal melanoma No radiation-related morbidity Visionpreservation Local tumor control Reduce metastasisrisk with early treatment Improve safetyand quality of life Treatment Goals In-office procedure Two injections (2 min. each) 30 min. apart 10-30 min. procedure Delivery viasuprachoroidal injection Light activation with standard ophthalmic laser Suprachoroidal Bel-sar (AU-011) is an investigational product candidate. The effectiveness and safety of bel-sar have not been established, and bel-sar is not approved for use in any jurisdiction.

Received fast track and orphan drug designations An SPA agreement indicates concurrence by the FDA that the design of the trial can adequately support a regulatory submission BCVA, best-corrected visual acuity; ETDRS, Early Treatment Diabetic Retinopathy Study; LBD, largest basal diameter; SPA, Special Protocol Assessment.ClinicalTrials.gov Identifier: NCT06007690; AU-011-301. Bel-sar for small choroidal melanoma or indeterminate lesions: Global phase 3 CoMpass trial now enrolling 15-month primary efficacy analysis 80 µg bel-sar treatment arm(n=40) 40 µg bel-sar treatment arm(n=20) Sham control arm (n=40) Participantswith small choroidal melanoma or indeterminate lesions Randomize 2:1:2 First key secondary endpoint Primary endpoint Time to tumor progression Increase in tumor thickness ≥0.5 mm or ≥1.5 mm in LBD Time to composite endpoint: Tumor progression or visual acuity failure ≥15 decrease in ETDRS-BCVA letter score from baseline Increase in tumor thickness ≥0.5 mm or ≥1.5 mm in LBD OR Target enrollment ~100 participants globally Anticipated sites in North America, Europe, Middle East and Asia-Pacific Regions

Phase 2 end of study data represented using planned phase 3 endpoints Kaplan-Meier analysis simulation of time-to-event Study duration 12 months. Participants either had an event or were censored at the last visit; some had their Week 52 visit after 365 days. Any events at the final visit are assigned to the actual time of that visit. Log-rank test p-value based on unsimulated original Kaplan-Meier curves. BCVA, best-corrected visual acuity; ETDRS, Early Treatment Diabetic Retinopathy Study; LBD, largest basal diameter. ClinicalTrials.gov Identifiers: NCT04417530; AU-011-202 (phase 2); NCT06007690; AU-011-301 (phase 3).Data on file, Aura Biosciences. Survival probability P = 0.0005 Time to tumor progression Time to composite endpoint Change from baseline in thickness ≥0.5 mm; or in LBD ≥1.5 mm confirmed by at least one repeat assessment Therapeuticn=10 Subtherapeutic n=10 Time to tumor progression or vision acuity failure (≥15 letter loss in ETDRS-BCVA), whicheveroccurs earlier 0.0 0.2 0.4 0.6 0.8 1.0 + Censored 0.0 0.2 0.4 0.6 0.8 1.0 0 100 200 300 400 500 P = 0.0008 Survival probability 0 100 200 300 400 500 + Censored Treatment duration (days) Treatment duration (days)

Bel-sar opportunities in ocular oncology represent a multi-billion-dollar addressable market With only ~100 ocular oncologists in the US/EU,a global launch may be accomplished with a small(<20) field-based team aIncludes conjunctival melanoma, primary acquired melanosis, squamous cell carcinoma and ocular surface squamous neoplasia.1-5 1. Yu G-P et al. Am J Ophthalmol. 2003;135(6):800-6. 2. Triay E et al. Br J Ophthalmol. 2009;93(11):1524-8. 3. Newton R et al. Lancet. 1996;347(9013):1450-1. 4. Dalvin LA. Br J Ophthalmol. 2018;102(12):1728-1734. 5. Sun EC et al. Cancer Epidemiol Biomarkers Prev. 1997;6(2):73-7. 6. Epidemiology analysis for choroidal melanoma and choroidal metastasis by ClearView Healthcare Partners and Putman. 7. American Cancer Society. Key statistics for retinoblastoma. Available at: https://www.cancer.org/cancer/types/retinoblastoma/about/key-statistics.html. Accessed Sept 5, 2024. Bel-sar (AU-011) is an investigational product candidate. The effectiveness and safety of bel-sar have not been established, and bel-sar is not approved for use in any jurisdiction. Ocular surface cancers ~66,000 patients/year ~35,000/yra,1–5 Primary uveal melanoma ~11,000/yr6 Metastases to the choroid ~20,000/yr6 Retinoblastoma ~500/yr7 Ocular oncology franchise total addressable market (US/EU)
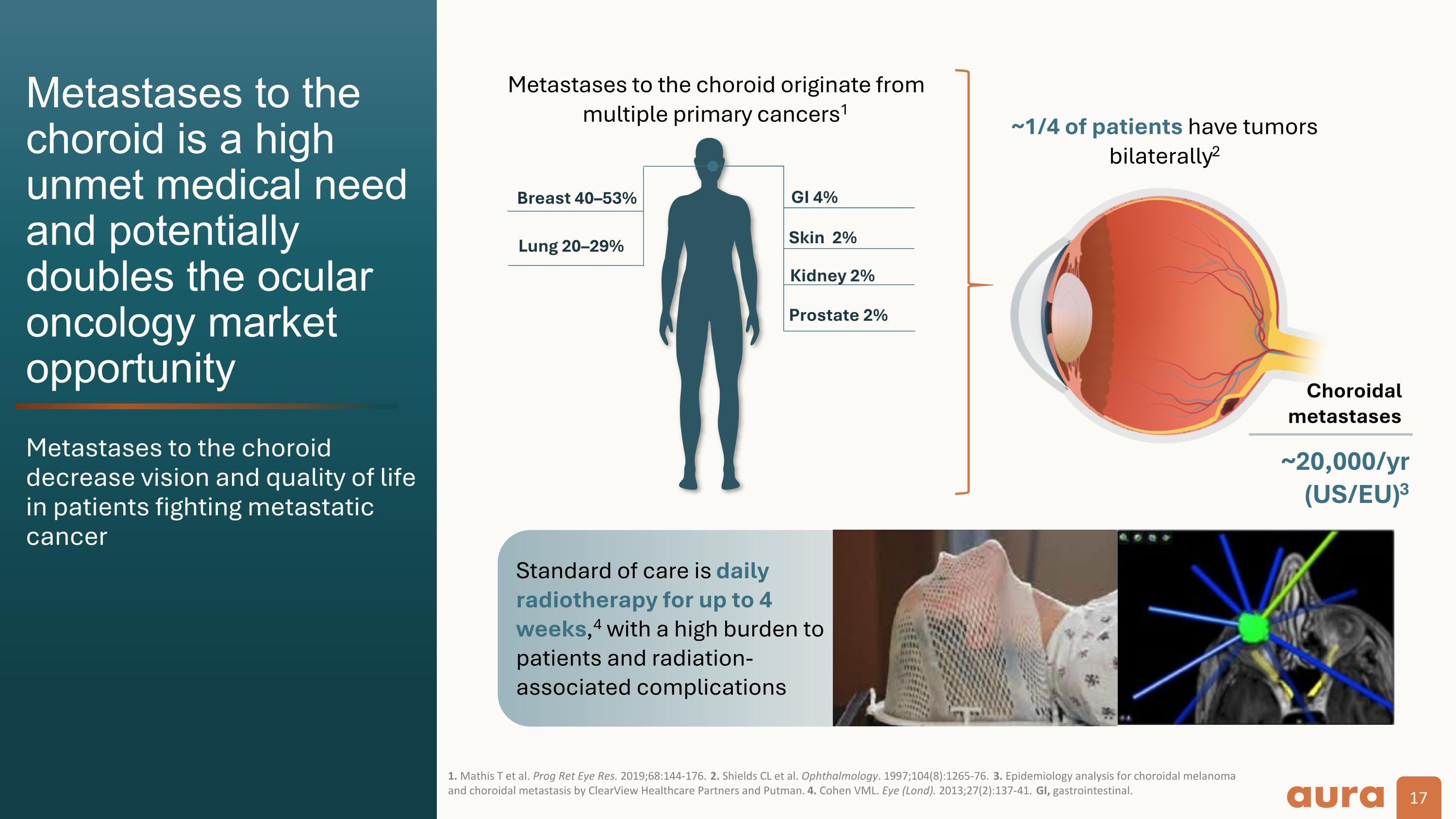
Metastases to the choroid is a high unmet medical need and potentially doubles the ocular oncology market opportunity Metastases to the choroid decrease vision and quality of life in patients fighting metastatic cancer 1. Mathis T et al. Prog Ret Eye Res. 2019;68:144-176. 2. Shields CL et al. Ophthalmology. 1997;104(8):1265-76. 3. Epidemiology analysis for choroidal melanoma and choroidal metastasis by ClearView Healthcare Partners and Putman. 4. Cohen VML. Eye (Lond). 2013;27(2):137-41. GI, gastrointestinal. Metastases to the choroid originate from multiple primary cancers1 ~1/4 of patients have tumors bilaterally2 Choroidal metastases ~20,000/yr (US/EU)3 Skin 2% Kidney 2% Breast 40–53% Lung 20–29% GI 4% Prostate 2% Standard of care is daily radiotherapy for up to 4 weeks,4 with a high burden to patients and radiation-associated complications

Highlights: Primary endpoint at one-month post-treatment; possibility to see tumor shrinkage and vision improvement *3+3 Design. Each cohort to have a minimum of 3 and a maximum of 6 patients **Simplified schema of study design. Metastases to the choroid: first sites activated StudyPopulation StudyObjectives Safety/dose-limiting toxicity Efficacy Change in tumor size Change in vision letter score Patients with unilateral, unifocal metastases to the choroid Breast or lung primary No changes in concurrent systemic medications planned Study Design (n=12*) Cohort 1 (N=3) 80µg 1 cycle Cohort 2 (N=3) 160µg 1 cycle Cohort 3 (N=3) 200µg 1 cycle Cohort 4 (N=3) 200µg 2 cycles <2 DLTs <2 DLTs <2 DLTs Cohort 3 (N=3) 200µg 1 cycle Cohort 4 (N=3) 200µg 2 cycles ≥2 DLTs

Urologic Oncology Bel-sar target indications: Intermediate-risk NMIBC | High-risk NMIBC

20 Bel-sar seeks to redefine the treatment of bladder cancer with a novel and disruptive approach

1. GLOBOCAN 2022. Bladder. Available at: https://gco.iarc.who.int/media/globocan/factsheets/cancers/30-bladder-fact-sheet.pdf. [Accessed October 1, 2024]. 2. Sung H, et al. CA Cancer J Clin. 2021;71(3):209–49. 3. Burger M, et al. Eur Urol. 2013;63(2):234–41. 4. Flaig TW, et al. J Natl Compr Canc Netw. 2018;16(9):1041–53. 5. Clark O, et al. Pharmacoecon Open. 2024 Aug 18. doi: 10.1007/s41669-024-00512-8. [Online ahead of print]. 6. Lamm DL, et al. J Urol. 2000;163(4):1124-9. 7. Shore ND, et al. Urol Oncol. 39(10):642–63. 8. Shalata AT, et al. Cancers (Basel). 2022;14(20):5019. BCG, Bacillus Calmette-Guerin; MIBC, muscle-invasive bladder cancer; NMIBC, non-muscle-invasive bladder cancer; QoL, quality of life; TURBT, transurethral resection of bladder tumor. Bladder cancer: High unmet medical need for function-preserving organ-sparing therapies 9th most commoncancer worldwide1 >$6 billion Annual costof treatment in US5 One of the highest lifetime treatment costs of all cancers Conventional bladder cancer treatments are suboptimal Short- and long-term side effects Considerable impact on QoL Inadequate efficacy Multiple TURBT surgeries Disease progression/metastasis Loss of bladder/cystectomy MIBC25% NMIBC 75% Ranked 13th for mortality1 21 21 The majority of bladder cancer patients present with NMIBC3 ~70-80% of patients with NMIBC develop recurrence after treatment8 NMIBC MIBC >600,000 614,298 diagnosed in 20221(>7% increase from 2020)1,2 cases/year globally1 84% Patients are receiving fewer courses of BCG due to global shortage7 of patients do not complete a full course of BCG treatment6
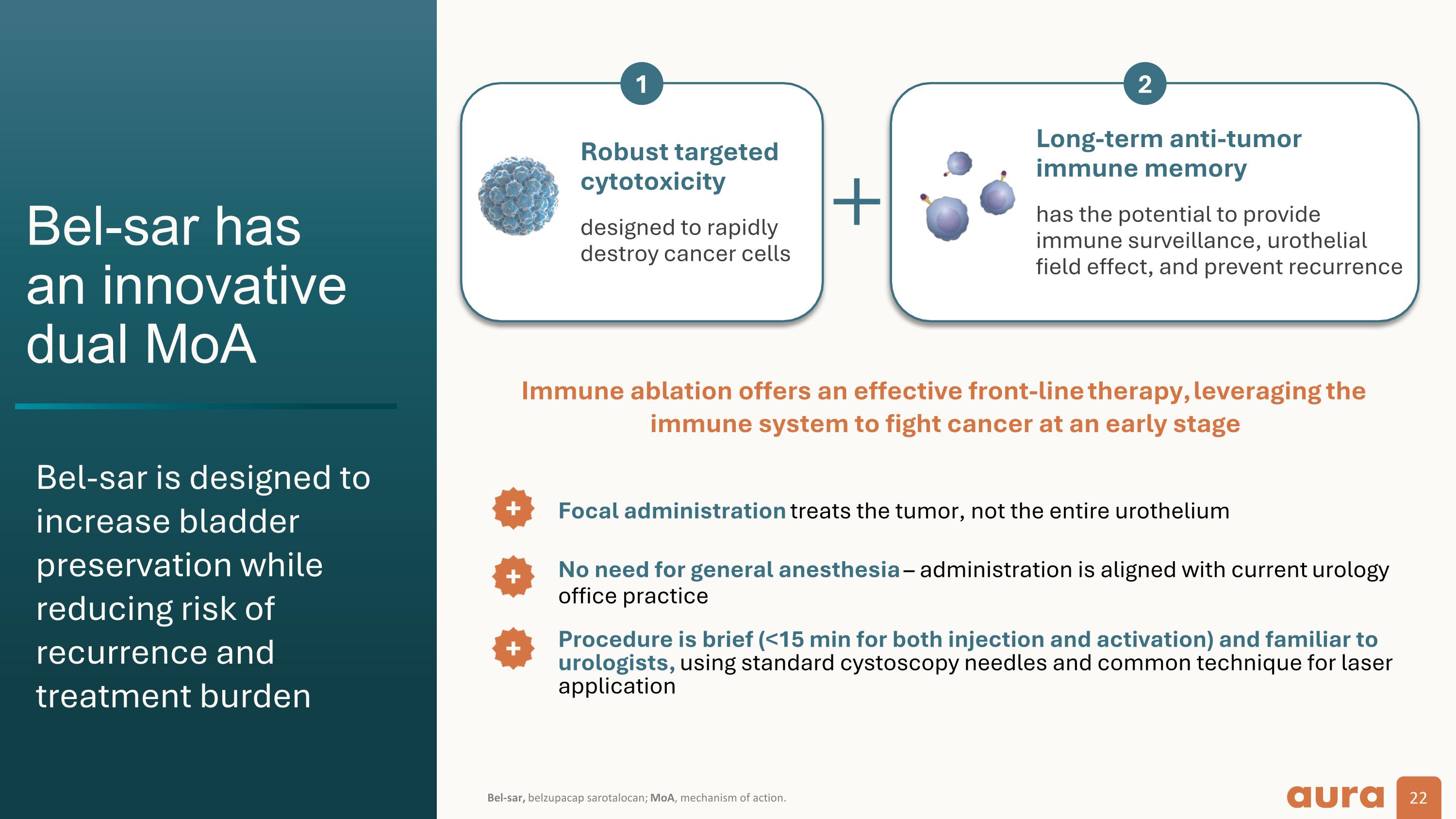
Bel-sar hasan innovative dual MoA Long-term anti-tumorimmune memory has the potential to provide immune surveillance, urothelial field effect, and prevent recurrence Robust targeted cytotoxicity designed to rapidly destroy cancer cells 1 2 Focal administration treats the tumor, not the entire urothelium Immune ablation offers an effective front-line therapy, leveraging the immune system to fight cancer at an early stage No need for general anesthesia – administration is aligned with current urology office practice Bel-sar, belzupacap sarotalocan; MoA, mechanism of action. Procedure is brief (<15 min for both injection and activation) and familiar to urologists, using standard cystoscopy needles and common technique for laser application Bel-sar is designed to increase bladder preservation while reducing risk of recurrence and treatment burden

~80,000 ~20,000 Low grade – low & intermediate risk High-risk papillary disease High-risk CIS – BCG unresponsive BCG Intravesical chemotherapy ~4,000 TURBT recurrence Intravesical gene therapy Systemic immunotherapy TURBT recurrence Adjuvant therapy Adjuvant therapy Intravesical immunotherapy BCG Intravesical chemotherapy Adjuvant therapy Cystectomy Disease progression Recurrencea Prevalence (US patients)1–3 a42–84% of low-grade IR patients develop recurrence.4,5 1. Holzbeierlein JM et al. J Urol. 2024;212(1):3–10. 2. Holzbeierlein JM et al. J Urol. 2024 Apr;211(4):533–58. 3. Internal Aura epidemiology of market size; data on file. 4. Shalata AT, et al. Cancers (Basel). 2022;14(20):5019. 5. van Rhijn BWG, et al. Eur Urol. 2009;56(3):430–42. BCG, Bacillus Calmette-Guérin; CIS, carcinoma in situ; TURBT, transurethral resection of bladder tumor. Current treatment paradigm based on upfront resection leads to recurrence Front line Front line High recurrence rate leads to multiple surgeries and burdensome adjuvant treatment intervention

A, adjuvant treatment; APC, antigen-presenting cell; B, bel-sar; bel-sar, belzupacap sarotalocan; DAMPs, damage-associated molecular patterns; M, month; MOA, mechanism of action; NIR, near-infrared; SoC, standard-of-care; T, TURBT; TURBT, transurethral resection of bladder tumor. Bel-sar shifts the treatment paradigm from resection-based toimmune-ablative front-line treatment Direct tumor cell killing + long-term anti-tumor immunity B A A A T A A A A A A A A A A A A M0 M3 M6 M12 M0 T High treatment burden (potential multiple surgeries) High risk of recurrence Anti-tumor immunity has the potential to provide immune surveillance and long-term protection Current SoC: TURBT + adjuvant treatment Bel-sar has an immune-mediated MoA NIR light bel-sar injection Necrotic tumor cells IMMUNE ACTIVATION DAMPS and neoantigens Activation of APCs Presentation of neoantigens to T cells T cell trafficking and proliferation TURBT followed by multiple adjuvant treatments (maintenance for up to 12 months or longer) B TURBT Tumor cells No tumor cells+immune surveillance
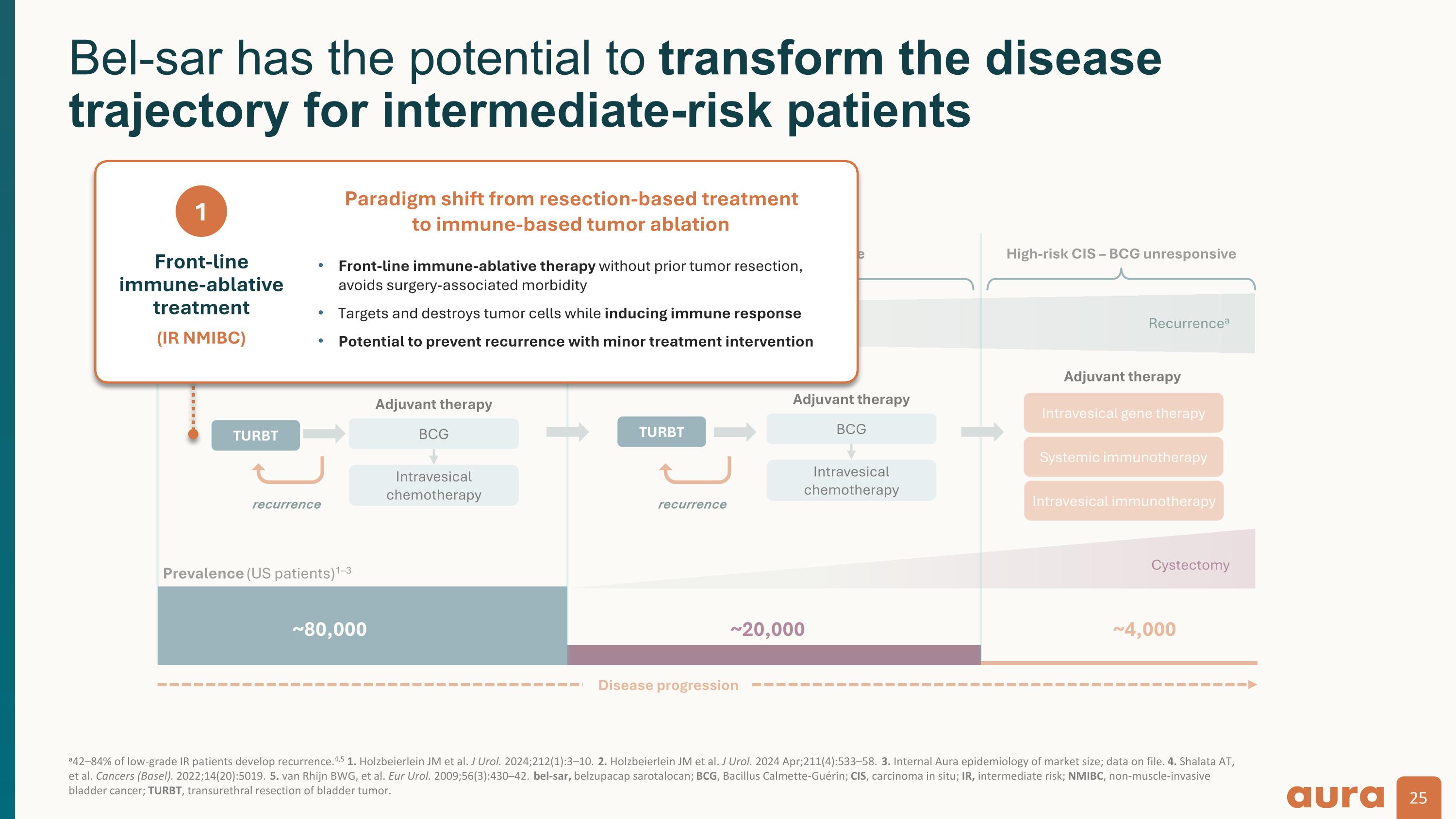
~80,000 ~20,000 Low grade – low & intermediate risk High-risk papillary disease High-risk CIS – BCG unresponsive BCG Intravesical chemotherapy ~4,000 TURBT recurrence Intravesical gene therapy Systemic immunotherapy TURBT recurrence Adjuvant therapy Adjuvant therapy Intravesical immunotherapy BCG Intravesical chemotherapy Adjuvant therapy Cystectomy Disease progression Recurrencea Prevalence (US patients)1–3 a42–84% of low-grade IR patients develop recurrence.4,5 1. Holzbeierlein JM et al. J Urol. 2024;212(1):3–10. 2. Holzbeierlein JM et al. J Urol. 2024 Apr;211(4):533–58. 3. Internal Aura epidemiology of market size; data on file. 4. Shalata AT, et al. Cancers (Basel). 2022;14(20):5019. 5. van Rhijn BWG, et al. Eur Urol. 2009;56(3):430–42. bel-sar, belzupacap sarotalocan; BCG, Bacillus Calmette-Guérin; CIS, carcinoma in situ; IR, intermediate risk; NMIBC, non-muscle-invasive bladder cancer; TURBT, transurethral resection of bladder tumor. Front-line immune-ablative treatment (IR NMIBC) Front-line immune-ablative therapy without prior tumor resection, avoids surgery-associated morbidity Targets and destroys tumor cells while inducing immune response Potential to prevent recurrence with minor treatment intervention 1 Bel-sar has the potential to transform the disease trajectory for intermediate-risk patients Paradigm shift from resection-based treatmentto immune-based tumor ablation

Bel-sar has potential as a standalone immune-ablative treatment or as a neoadjuvant to TURBT Immune-ablative approach could eliminate the need for TURBT, or be used prior to resection to improve treatment outcomes APC, antigen-presenting cell; bel-sar, belzupacap sarotalocan; DAMPs, damage-associated molecular patterns; HR, high-risk; IR, intermediate risk; LR, low-risk; NIR, near-infrared; NMIBC, non-muscle-invasive bladder cancer; TURBT, transurethral resection of bladder tumor. Immune-ablative treatment without TURBT (LR/IR NMIBC) 1 Neoadjuvant/multimodal therapy followed by TURBT (IR/HR NMIBC) 2 NIR light bel-sar injection Necrotic tumor cells IMMUNE ACTIVATION DAMPS and neoantigens Activation of APCs Presentation of neoantigens to T cells T cell trafficking and proliferation NIR light bel-sar injection Necrotic tumor cells IMMUNE ACTIVATION DAMPS and neoantigens Activation of APCs Presentation of neoantigens to T cells T cell trafficking and proliferation Necrotic tissue TURBT No tumor cells+immune surveillance No tumor cells+immune surveillance

~80,000 ~20,000 Low grade – low & intermediate risk High-risk papillary disease High-risk CIS – BCG unresponsive BCG Intravesical chemotherapy ~4,000 TURBT recurrence Intravesical gene therapy Systemic immunotherapy TURBT recurrence Adjuvant therapy Adjuvant therapy Intravesical immunotherapy BCG Intravesical chemotherapy Adjuvant therapy Cystectomy Disease progression Recurrencea Prevalence (US patients)1–3 a42–84% of low-grade IR patients develop recurrence.4,5 1. Holzbeierlein JM et al. J Urol. 2024;212(1):3–10. 2. Holzbeierlein JM et al. J Urol. 2024 Apr;211(4):533–58. 3. Internal Aura epidemiology of market size; data on file. 4. Shalata AT, et al. Cancers (Basel). 2022;14(20):5019. 5. van Rhijn BWG, et al. Eur Urol. 2009;56(3):430–42. bel-sar, belzupacap sarotalocan; BCG, Bacillus Calmette-Guérin; CIS, carcinoma in situ; HR, high risk; IR, intermediate risk; NMIBC, non-muscle-invasive bladder cancer; TURBT, transurethral resection of bladder tumor. Bel-sar has the potential to transform the disease trajectory for high-risk patients Neoadjuvant/multimodal prior to TURBT (IR/HR NMIBC) Bel-sar before TURBT to shrink/eradicate tumors and generate T-cell mediated immunity Enables next-generation combination strategies (e.g., with checkpoint inhibitors) and could reduce need for adjuvant therapy Potential to reduce risk of recurrence and progression with minor intervention 2 Paradigm shift from resection-based + adjuvant treatments to immune-based neoadjuvant multimodal approach

Phase 1 data Phase 1 trial of bel-sar in bladder cancer

Bel-sar, belzupacap sarotalocan; TURBT, transurethral resection of bladder tumor. Clinicaltrials.gov identifier: NCT05483868; AU-011-102. Bel-sar is administered before scheduled biopsy and standard of care (SoC) TURBT Day 1 Cystoscopy + biopsy bel-sar injection Day 2 Cystoscopy Laser light activation Day 9 ± 1 (Cohort A)Day 14+7 (Cohort B+C) Day 56 ± 7 End of follow-up Pathology specimen Pathology specimen Final efficacy evaluation Final safety evaluation Treatment Phase: Feasibility and mechanism of action Follow-up Phase: Safety Clinical response data up to 21 days; safety data up to 56 days SoC TURBT Final Cystoscopy

Bel-sar, belzupacap sarotalocan; NMIBC, non-muscle-invasive bladder cancer; TURBT, transurethral resection of bladder tumor.Clinicaltrials.gov identifier: NCT05483868; AU-011-102. Phase 1 trial of bel-sar for bladder cancer designed to evaluate safety, feasibility, and mechanism of action Safety Review Board completed after each cohort. Patients followed for safety after TURBT to 56 days. Total 100 µg NMIBC (N=5) 50 µg at tumor base 50 µg within lamina propria Drug only (No light) Total 100 µg NMIBC (N=4) 50 µg at tumor base 50 µg within lamina propria Cohort A: Drug + light Total 100 µg NMIBC (N=3) 100 µg at tumor base Cohort B: Drug + light Study objectives Safety & dose-limiting toxicity Focal distributionof bel-sar Feasibility of technique Focalnecrosis Markers ofimmune activation Histopathological assessment completed at time of standard of care TURBT Part 1 (n=5) Bel-sar + focal light activation Single dose window of opportunity study in NMIBC all-comers Bel-sar alone Part 2 (n=~10) Cohort C: Drug + light Total 200 µg NMIBC (N=3) 200 µg at tumor base
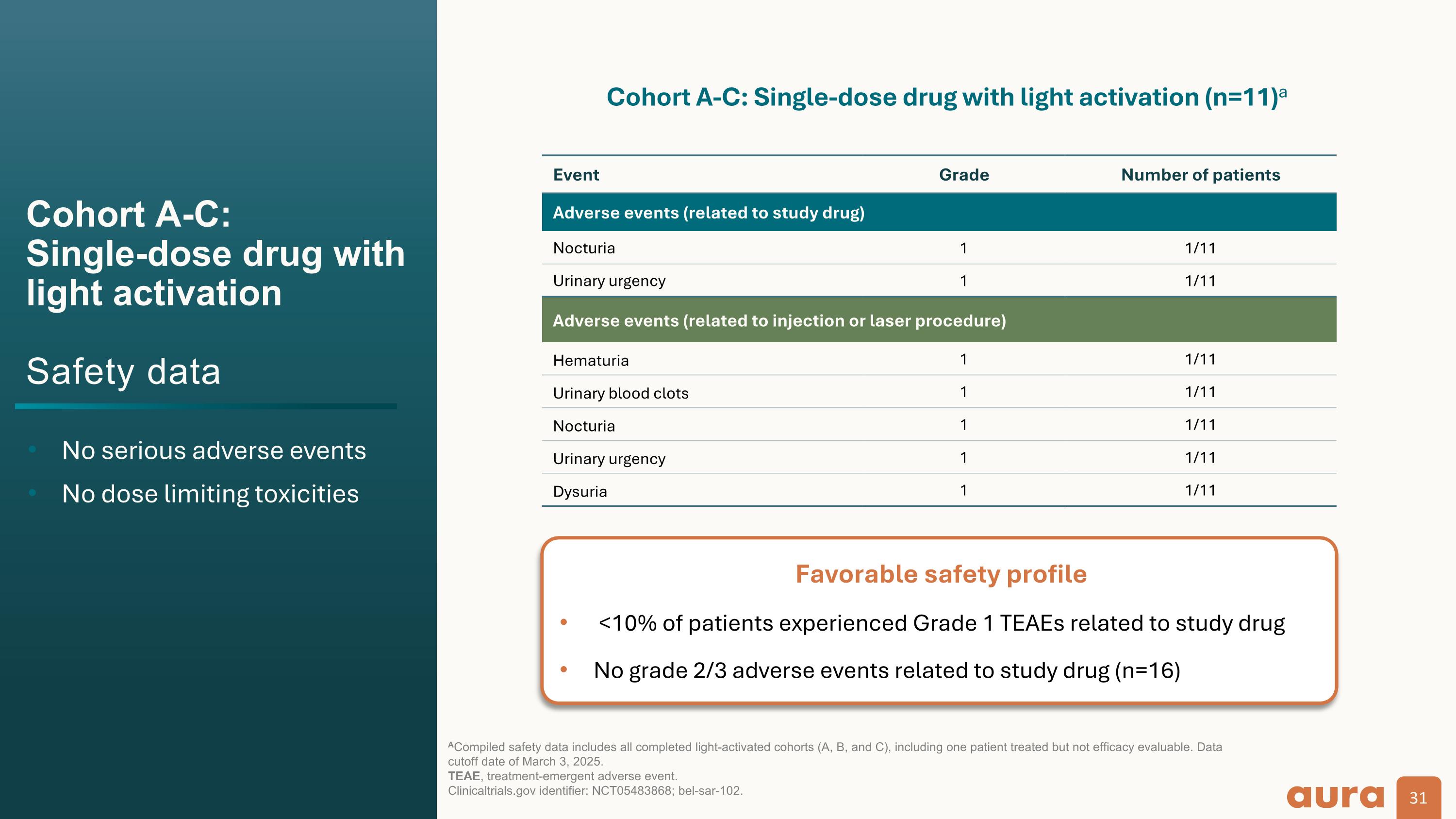
Cohort A-C:Single-dose drug with light activationSafety data No serious adverse events No dose limiting toxicities ACompiled safety data includes all completed light-activated cohorts (A, B, and C), including one patient treated but not efficacy evaluable. Data cutoff date of March 3, 2025.TEAE, treatment-emergent adverse event.Clinicaltrials.gov identifier: NCT05483868; bel-sar-102. Event Grade Number of patients Adverse events (related to study drug) Nocturia 1 1/11 Urinary urgency 1 1/11 Adverse events (related to injection or laser procedure) Hematuria 1 1/11 Urinary blood clots 1 1/11 Nocturia 1 1/11 Urinary urgency 1 1/11 Dysuria 1 1/11 Cohort A-C: Single-dose drug with light activation (n=11)a Favorable safety profile <10% of patients experienced Grade 1 TEAEs related to study drug No grade 2/3 adverse events related to study drug (n=16)
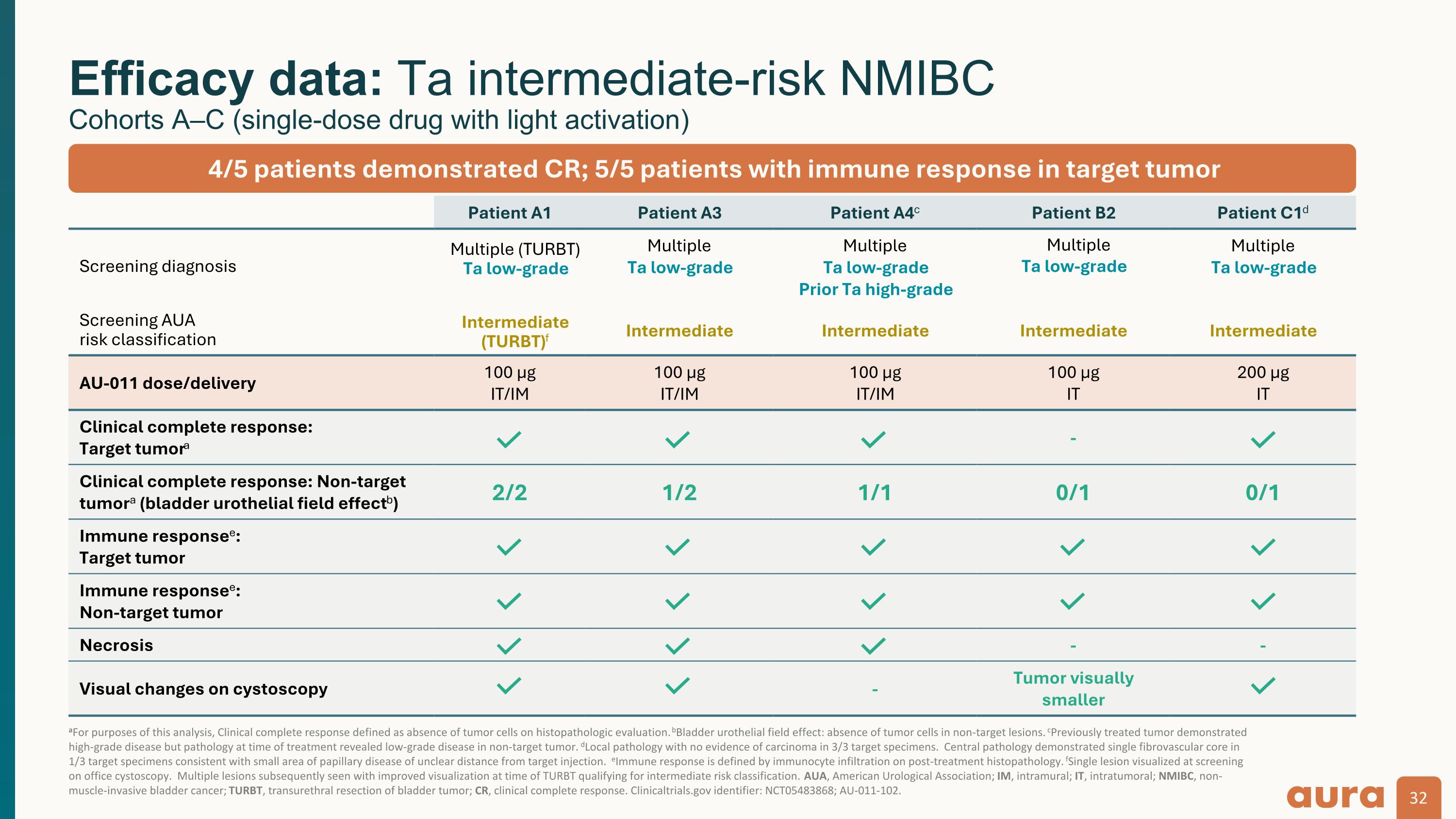
aFor purposes of this analysis, Clinical complete response defined as absence of tumor cells on histopathologic evaluation. bBladder urothelial field effect: absence of tumor cells in non-target lesions. cPreviously treated tumor demonstrated high-grade disease but pathology at time of treatment revealed low-grade disease in non-target tumor. dLocal pathology with no evidence of carcinoma in 3/3 target specimens. Central pathology demonstrated single fibrovascular core in 1/3 target specimens consistent with small area of papillary disease of unclear distance from target injection. eImmune response is defined by immunocyte infiltration on post-treatment histopathology. fSingle lesion visualized at screening on office cystoscopy. Multiple lesions subsequently seen with improved visualization at time of TURBT qualifying for intermediate risk classification. AUA, American Urological Association; IM, intramural; IT, intratumoral; NMIBC, non-muscle-invasive bladder cancer; TURBT, transurethral resection of bladder tumor; CR, clinical complete response. Clinicaltrials.gov identifier: NCT05483868; AU-011-102. Efficacy data: Ta intermediate-risk NMIBCCohorts A–C (single-dose drug with light activation) Patient A1 Patient A3 Patient A4c Patient B2 Patient C1d Screening diagnosis Multiple (TURBT) Ta low-grade Multiple Ta low-grade Multiple Ta low-grade Prior Ta high-grade Multiple Ta low-grade Multiple Ta low-grade Screening AUArisk classification Intermediate (TURBT)f Intermediate Intermediate Intermediate Intermediate AU-011 dose/delivery 100 µgIT/IM 100 µgIT/IM 100 µgIT/IM 100 µgIT 200 µgIT Clinical complete response:Target tumora - Clinical complete response: Non-target tumora (bladder urothelial field effectb) 2/2 1/2 1/1 0/1 0/1 Immune responsee:Target tumor Immune responsee: Non-target tumor Necrosis - - Visual changes on cystoscopy - Tumor visually smaller 4/5 patients demonstrated CR; 5/5 patients with immune response in target tumor

aClinical complete response defined as absence of tumor cells on histopathologic evaluation. bBladder urothelial field effect: absence of tumor cells in non-target lesions. cImmune response is defined by immunocyte infiltration on post-treatment histopathology. dTwo tumors in target tumor field with 1/2 tumors with clinical complete response. BCG failure qualifying as high risk by AUA criteria. AUA, American Urological Association; BCG, Bacillus Calmette-Guerin; NMIBC, non-muscle-invasive bladder cancer; CR, clinical complete response; IM, intramural; IT, intratumoral. Clinicaltrials.gov identifier: NCT05483868; AU-011-102. Efficacy data: Ta high-risk NMIBCCohorts A–C (single-dose drug with light activation) Patient A2 Patient B1 Patient B3 Patient C2 Patient C3d Screening diagnosis Single Ta high-grade Multiple Ta high-grade Single Ta high-grade Multiple Ta high-grade Multiple Ta low-grade Prior Ta high-grade Screening AUArisk classification High High High High High (BCG Failure) AU-011 dose/delivery 100 µgIT/IM 100 µgIT 100 µgIT 200 µgIT 200 µgIT Clinical complete response: Target tumora - - - - Clinical complete response: Non-target tumora (bladder urothelial field effectb) NA 0/1 NA NA 1/3 Immune responsec: Target tumor Immune responsec: Non-target tumor NA NA NA Necrosis - - - - Visual changes on cystoscopy Tumor visually smaller Tumor visually smaller - Tumor visually smaller 1/5 patients demonstrated CR; 5/5 patients with immune response in target tumor

Cohort A:Single-dose drug with light activation Patient A372-year-old Hispanic male Screening diagnosis: (2024) Multiple Ta low-grade (<3 cm) No CIS Screening AUA risk classification: Intermediate Initial diagnosis: (2019) Ta high-grade <3 cm No CIS Intermediate risk Prior TURBT: 2019, 2020 (x2), 2021 (x2), 2023 Prior adjuvant therapies: BCG induction and maintenance (2020-2021) AUA, American Urological Association; BCG, Bacillus Calmette-Guerin; CIS, carcinoma in situ; TURBT, transurethral resection of bladder tumor.Clinicaltrials.gov identifier: NCT05483868; AU-011-102. Clinical complete response visualized at time of TURBT confirmed with histopathologic evaluation Biopsy bel-sar injection Pre-injection/pre-biopsy appearance of tumor on office cystoscopy Post-injection edema andecchymosis at injection site
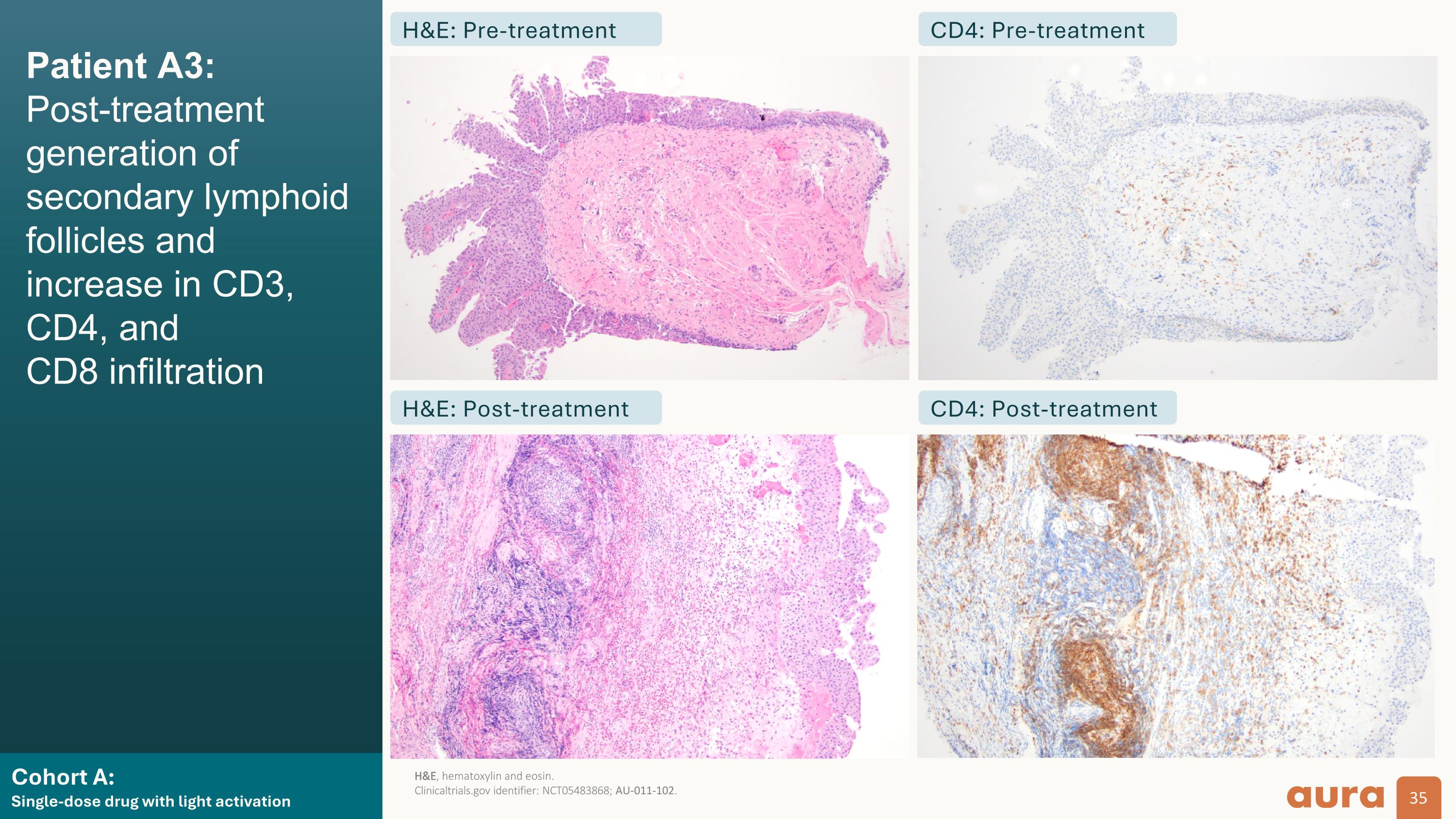
Cohort A:Single-dose drug with light activation Patient A3:Post-treatment generation of secondary lymphoid follicles and increase in CD3, CD4, andCD8 infiltration H&E: Pre-treatment H&E: Post-treatment CD4: Pre-treatment CD4: Post-treatment H&E, hematoxylin and eosin.Clinicaltrials.gov identifier: NCT05483868; AU-011-102.

Multiplex Immunofluorescence: Patient A3 (Intermediate-Risk NMIBC) TLS Not Present in Lesion Prior to Treatment Mature Tertiary Lymphoid Structures (TLS) in Target (Treated) Lesion: Active Immunosurveillance After Bel-sar Treatment CD3: T cells CD20: B cells CD23: Follicular Dendritic Cells (FDC) (Found in B cell follicles, only present in mature TLS) PNAd: Peripheral Node Addressin (Stains for high endothelial venules, evidence of lymphocyte trafficking from periphery)

Early Tertiary Lymphoid Structures (TLS) in Distant Non-Target (Non-Treated) Lesion: Urothelial Immune Field Effect After Bel-sar Treatment Multiplex Immunofluorescence: Patient A3 (Intermediate-Risk NMIBC) CD3: T cells CD20: B cells CD23: Follicular Dendritic Cells (FDC) (Found in B cell follicles, only present in mature TLS) PNAd: Peripheral Node Addressin (Stains for high endothelial venules, evidence of lymphocyte trafficking from periphery)

Light-activated cohorts (A–C) after single, low-dose of bel-sar Clinical complete responses and immune responses demonstrated induction of effector immunity, relief from immunosuppression, and development of active immunosurveillance aTotal of 7 patients with non-target tumors. bOrganized aggregates of immune cells.Bel-sar, belzupacap sarotalocan; MOA, mechanism of action.Clinicaltrials.gov identifier: NCT05483868; AU-011-102. 100% (10/10) of patients showed target tumor infiltration of effector CD8+ T and CD4+ cells as early as 7 days after laser activation 100% (11/11) of non-target tumorsa showed T cell infiltration, supportive of a bladder urothelial field effect Focal eosinophilic infiltration was observed in target tumors in 60% (6/10) of patients. 9% (1/11) of non-target tumors showed eosinophilic infiltration, supportive of a local innate immune response to tumor necrosis Generation of lymphoid folliclesb was observed in target tumors in 80% (8/10) of patients, supportive of a local adaptive immune response
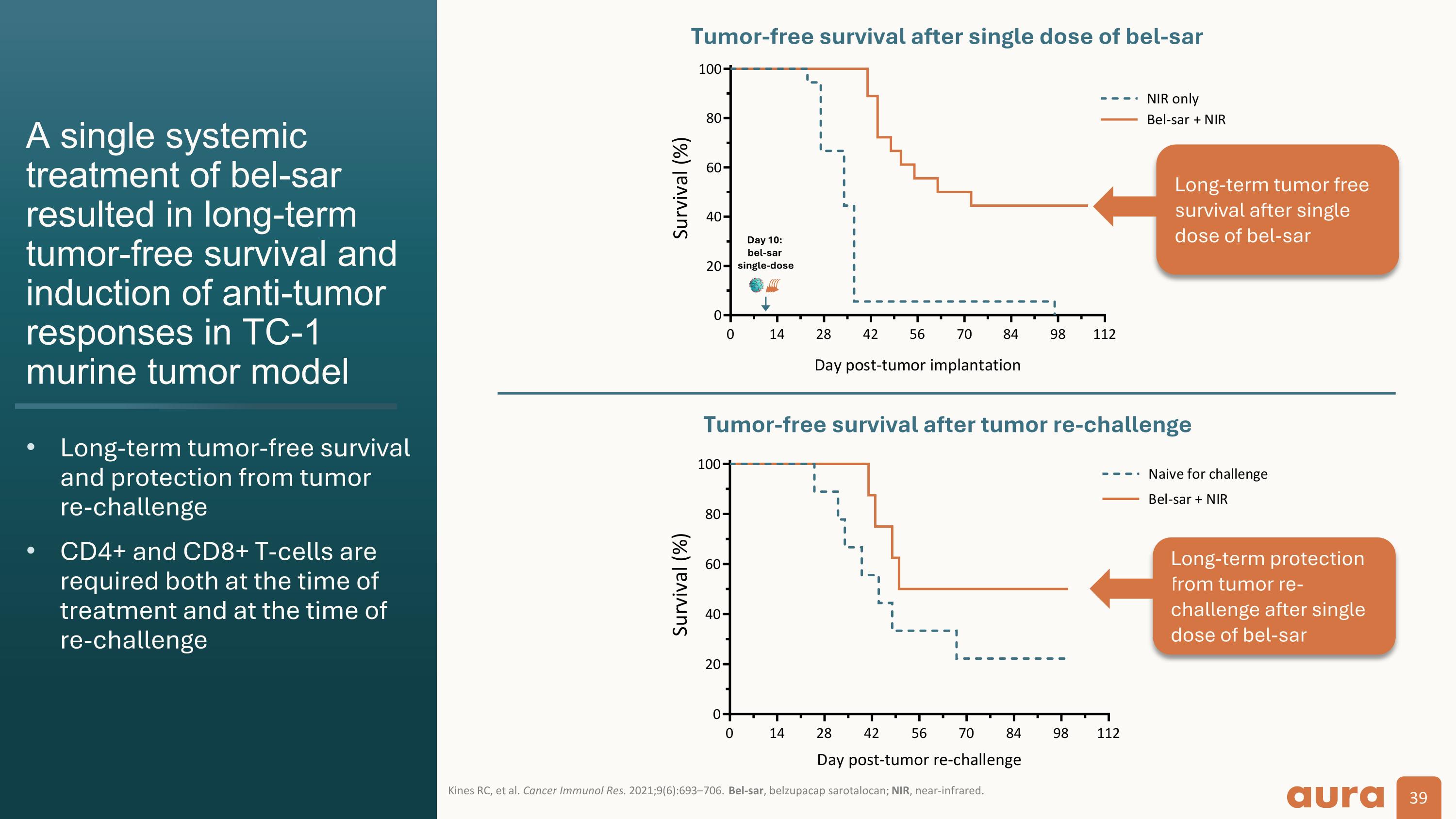
A single systemic treatment of bel-sar resulted in long-term tumor-free survival and induction of anti-tumor responses in TC-1 murine tumor model Long-term tumor-free survival and protection from tumorre-challenge CD4+ and CD8+ T-cells are required both at the time of treatment and at the time of re-challenge Kines RC, et al. Cancer Immunol Res. 2021;9(6):693–706. Bel-sar, belzupacap sarotalocan; NIR, near-infrared. Tumor-free survival after tumor re-challenge Day 10: bel-sar single-dose Long-term protection from tumor re-challenge after single dose of bel-sar Long-term tumor free survival after single dose of bel-sar Tumor-free survival after single dose of bel-sar
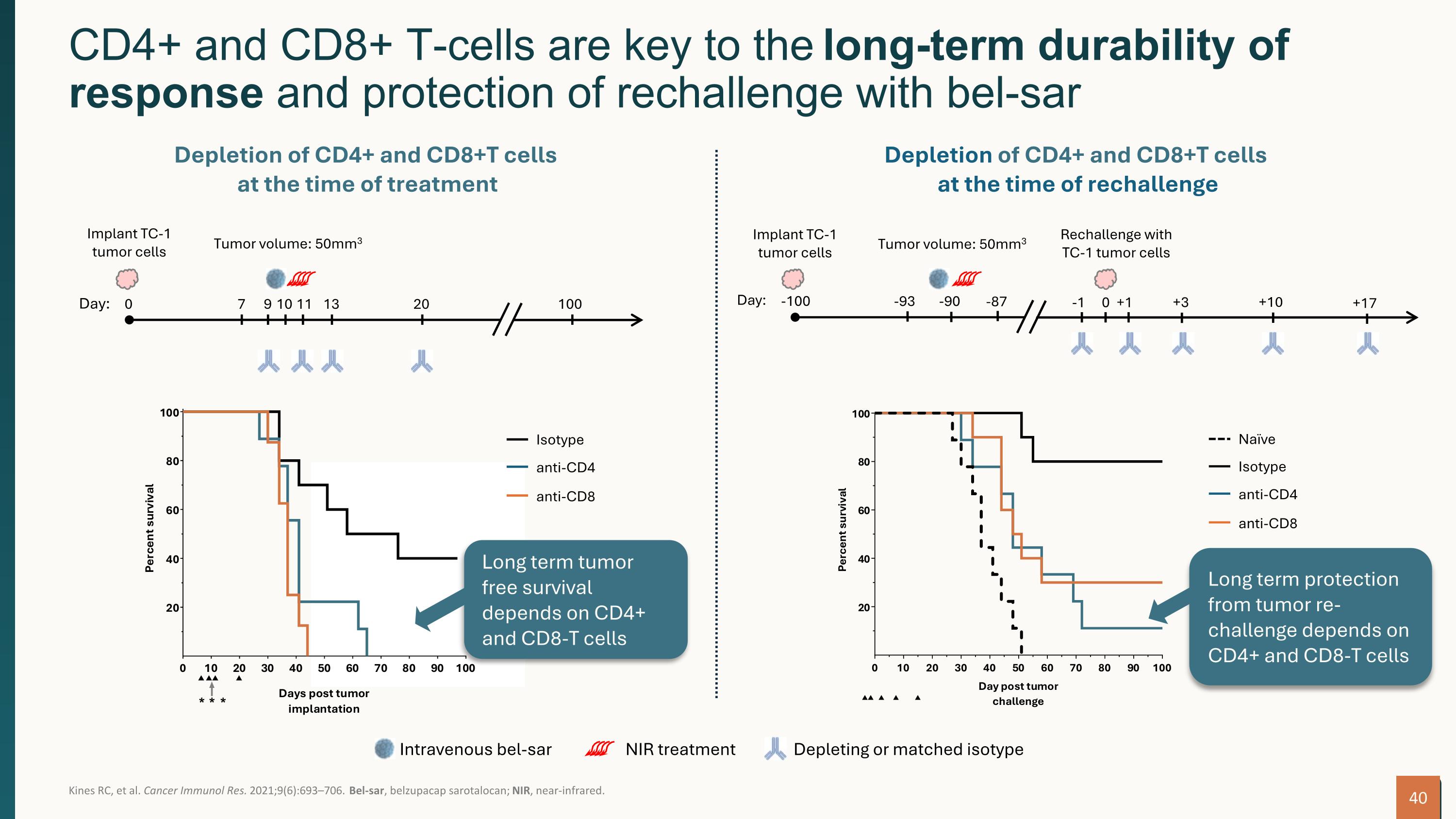
Kines RC, et al. Cancer Immunol Res. 2021;9(6):693–706. Bel-sar, belzupacap sarotalocan; NIR, near-infrared. CD4+ and CD8+ T-cells are key to the long-term durability of response and protection of rechallenge with bel-sar +1 9 11 Day: 0 100 Implant TC-1 tumor cells Tumor volume: 50mm3 7 10 13 20 Day: -100 0 Implant TC-1 tumor cells Rechallenge with TC-1 tumor cells Tumor volume: 50mm3 -93 -90 -87 +10 -1 +17 +3 Depletion of CD4+ and CD8+T cells at the time of treatment Depletion of CD4+ and CD8+T cells at the time of rechallenge Depleting or matched isotype Intravenous bel-sar NIR treatment Isotype anti-CD4 anti-CD8 Isotype anti-CD4 anti-CD8 Naïve Long term protection from tumor re-challenge depends on CD4+ and CD8-T cells Long term tumor free survival depends on CD4+ and CD8-T cells

Phase 1b/2 trial of bel-sar in non-muscle invasive bladder cancer

Paradigm-shifting treatment approach Treat the tumor first to generate cell-mediated immunity (CMI) BCG, Bacillus Calmette-Guérin; bel-sar, belzupacap sarotalocan; CMI, cell-mediated immunity; MIBC, muscle-invasive bladder cancer; NMIBC, non-muscle-invasive bladder cancer; TURBT, transurethral resection of bladder tumor. Neoadjuvant/multimodal(+ TURBT) Treat tumor with bel-sar firstahead of TURBT Immune-ablative(-TURBT) Treat tumor with bel-sar firstand avoid the need for TURBT Value proposition: Prevent recurrence and progression by treating the tumor first and generating CMI Avoid multiple cycles of adjuvant treatments (e.g., BCG, chemotherapy) Office-based procedure Patient population: Intermediate-risk and high-risk NMIBC patients; potential to expand to MIBC Value proposition: Prevent recurrence and progression by treating the tumor and generating CMI Avoid surgery (TURBT) and general anesthesia Office-based procedure Patient population: Intermediate-risk NMIBC patients

D, day; FU, follow-up; inj, injection; las, laser; M, month; W, week; NMIBC, non-muscle-invasive bladder cancer, .Clinicaltrials.gov identifier: NCT05483868; AU-011-102. Each cycle = 2 weeks Phase 1b/2 treatment schedule in intermediate and high-risk NMIBC patients Immune ablative design: Intermediate Risk Patients D1 D2 D15a D16 8W 3M FU 6M FU 9M FU 12M FU Cycle 1 Cycle 2 Cystoscopy as clinically indicated Response assessments inj. las. inj. las. V5 V6 V7 V8 1st treatment 2nd treatment V1 V2 V3 V4 Accelerated neoadjuvant design: Intermediate and High-Risk Patients D1 D2 D15a D16 2W TURBT Cycle 1 Cycle 2 inj. las. inj. las. V5 1st treatment 2nd treatment V1 V2 V3 V4 3M FU 6M FU 9M FU 12M FU Response assessments V6 V7 V8 V9 Established Regulatory Endpoints to Assess Durability of Response at 3 and 12 months
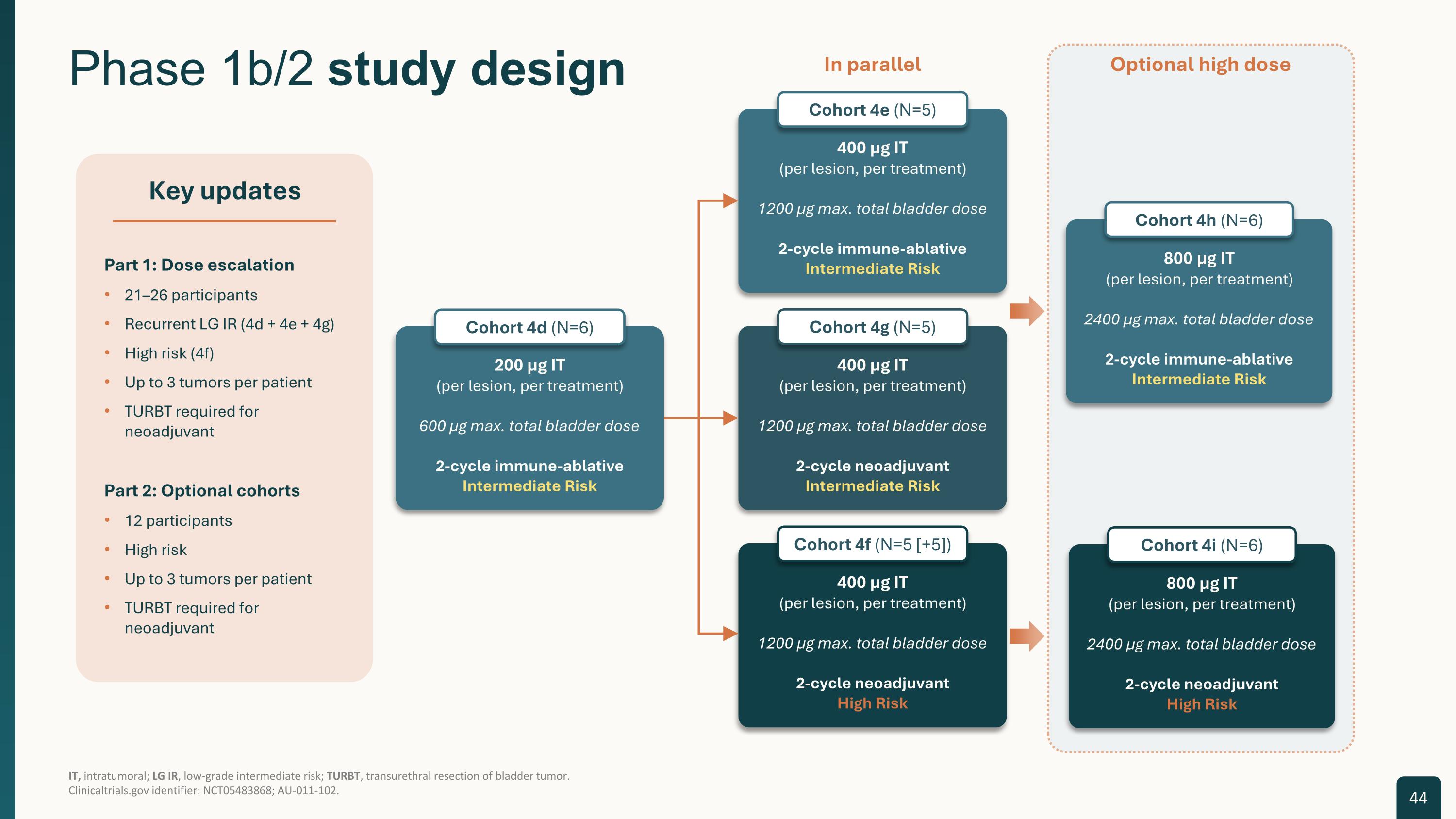
IT, intratumoral; LG IR, low-grade intermediate risk; TURBT, transurethral resection of bladder tumor.Clinicaltrials.gov identifier: NCT05483868; AU-011-102. Phase 1b/2 study design Key updates Part 1: Dose escalation 21–26 participants Recurrent LG IR (4d + 4e + 4g) High risk (4f) Up to 3 tumors per patient TURBT required for neoadjuvant Part 2: Optional cohorts 12 participants High risk Up to 3 tumors per patient TURBT required for neoadjuvant 44 200 µg IT(per lesion, per treatment) 600 µg max. total bladder dose 2-cycle immune-ablative Intermediate Risk Cohort 4d (N=6) 400 µg IT(per lesion, per treatment) 1200 µg max. total bladder dose 2-cycle immune-ablative Intermediate Risk Cohort 4e (N=5) Optional high dose 800 µg IT(per lesion, per treatment) 2400 µg max. total bladder dose 2-cycle immune-ablative Intermediate Risk Cohort 4h (N=6) 400 µg IT(per lesion, per treatment) 1200 µg max. total bladder dose 2-cycle neoadjuvant High Risk Cohort 4f (N=5 [+5]) 400 µg IT(per lesion, per treatment) 1200 µg max. total bladder dose 2-cycle neoadjuvant Intermediate Risk Cohort 4g (N=5) In parallel 800 µg IT(per lesion, per treatment) 2400 µg max. total bladder dose 2-cycle neoadjuvant High Risk Cohort 4i (N=6)

BCG, Bacillus Calmette-Guérin; Bel-sar, belzupacap sarotalocan; CIS, carcinoma in situ; MIBC, muscle-invasive bladder cancer; MIBC, muscle-invasive bladder cancer; NMIBC, non-muscle-invasive bladder cancer; TURBT, transurethral resection of bladder tumor. 45 Targeted cytotoxicity+ cell mediated anti-tumor immunity Active immunosurveillance Urothelial field effect Dual Mechanism of Action Transformative Clinical Impact Early clinical activity demonstrated across the disease spectrum Intermediate to high-risk NMIBC patients BCG-unresponsive patients Potential in additional indications (e.g. MIBC) Broad Market Opportunity Bel-sar seeks to redefine the treatment of bladder cancer with a novel and disruptive approach Front-line approach Immediate application in clinic Does not precludedownstream therapies Reduces total treatment burden Cell-mediated immunity has potential to generatelong-term durable responses

1. ClearView & Putnam & Assoc. Epidemiology Analysis Choroidal Melanoma and Choroidal Metastasis. FDA, United States Food and Drug Administration. NMIBC, non-muscle-invasive bladder cancer. Bel-sar (AU-011) is an investigational product candidate. The effectiveness and safety of bel-sar have not been established, and bel-sar is not approved for use in any jurisdiction. Company highlights Cash expected to fund operations into 2H 2026 Experienced leadership team across functions Corporate Ocular Oncology Therapeutic Area Primary uveal melanoma Global phase 3 CoMpass trial actively enrolling Special Protocol Assessment (SPA) agreement with FDA Phase 3 assumptions supported bypositive phase 2 end of study data Metastases to the choroid Phase 2 trial sites activated with patients in pre-screening Initial data expected in 2025 This ocular oncology indication potentiallydoubles market opportunity1 Urologic Oncology Therapeutic Area Multiple clinical complete responses with single low dose in phase 1 NMIBC trial Initial phase 1b/2 data evaluating additional doses, treatment regimens, and early durability of response in NMIBC anticipated in 2025

Appendix Ocular Oncology

Goal: To determine safety, optimal dose and therapeutic regimen with suprachoroidal administration One cycle = Doses on days 1, 8, and 15. a12 patients enrolled, 1 patient who discontinued after 1 cycle due to unrelated SAEs is not included in data analysis (n=11). bCohort 2: 2 participants were planned; third participant was additionally enrolled due to dose error in 1 participant.LBD, largest basal diameter; QW, every week; SAE, serious adverse event. ClinicalTrials.gov Identifier, NCT04417530: AU-011-202. Data on file, Aura Biosciences. Phase 2 trial of bel-sar for choroidal melanoma: Open-label, dose-escalation with suprachoroidal administration Trial design – 22 participants enrolled Patient population representative of early-stage disease: Small choroidal melanoma and indeterminate lesions Endpoints Tumor progression Growth in tumor height ≥0.5 mm or ≥1.5 mm in LBD relative to baseline Visual acuity loss ≥15 letters decrease from baseline Tumor thickness growth rate Change in rate of growth of tumor thickness 1 dose:20 μg x 1 laser 1 dose:40 μg x 1 laser 1 dose:40 μg x 2 lasers 2 doses:40 μg x 2 lasers QW x 2 9 doses:80 μg x 2 lasers QW x 3,3 cycles Subtherapeutic regimens(N=10) 1–2 doses (n=9); 2 cycles (6 doses; n=1) Therapeutic regimen(N=11)a 3 cycles (9 doses) Cohort 1 (n=1) Cohort 2 (n=3b) Cohort 3 (n=2) Cohort 4 (n=3) Cohort 5 (n=3) Cohort 6 (n=10) 6–9 doses:40 μg x 2 lasers QW x 3,up to 3 cycles (20 µg) (40 µg) (40 µg) (80 µg) (240–360 µg) (720 µg) Total intended dose

Baseline characteristics All study participants aHigh risk for vision loss defined as tumor edge within either 3 mm of foveal center or 3 mm of optic disc edge. BCVA, best-corrected visual acuity; ETDRS, Early Treatment Diabetic Retinopathy Study; LBD, largest basal diameter. Data on file, Aura Biosciences. All patients (n=22) Female (%) 54.5 White, not Hispanic or Latino (%) 100 Subretinal fluid at screening (%) 100 Orange pigment at screening (%) 86.4 Documented growth prior to screening (%) 86.4(100% of therapeutic group) Mean age at screening (years, ± SD) 59.2 (±16.5) Mean baseline BCVA in study eye (ETDRS letters, ± SD) 83.2 (±7.2) Mean baseline LBD (mm, ± SD) 8.5 (±1.4) Mean baseline tumor thickness (mm, ± SD) 2.0 (±0.5) Mean tumor distance to closest vision-critical structure at screening (mm, ± SD) 2.0 (±2.3) Tumors at high risk for vision loss (%)a 73%(80% [8/10] of therapeutic group)

High local complete response rate at 12 months follow-up 80% tumor control ratea at12 months among the 10phase 3-eligible patientsin the 3-cycle cohorts aLocal complete response, or CR, in early-stage choroidal melanoma is described as tumor control and complete arrest of tumor growth by ocular oncologists.bOne participant with circumpapillary tumor that did not meet phase 3 criteria is not included.LBD, largest basal diameter. ClinicalTrials.gov Identifier, NCT04417530: AU-011-202. Data on file, Aura Biosciences. Participants with tumor control at 12 months, % Dose/ Regimen n Tumor control rate, % Subtherapeutic regimen ≤2 cycles 10 20% (2/10) Therapeutic regimen 3 cycles, phase 3-eligibleb 10 80% (8/10) Phase 3-eligible participants High tumor control rates with therapeutic regimen inphase 3-eligible patients with active growth Median dose (IQR): 140 µg(80160) 720 µg(390–720)

Rate of tumor growth ± SE, mm/yr P < 0.0001 Rate of tumor growth with bel-sar treatment In phase 3-eligible patients, the 3-cycle regimen resulted in cessation of growth among responders (N=8) Tumor thickness growth rates/slopes estimated using Mixed Models for Repeat Measures (MMRM); random intercept and slope model for Historical and Study periods. ClinicalTrials.gov Identifier, NCT04417530: AU-011-202. Data on file, Aura Biosciences. Post-treatment actual growth rate Untreated projected growth rate Pre-treatment actual growth rate

Vision loss threshold(−15 letters) Populations Patients (n) Vision failuresb (n) Vision preservation rate (%) All dose cohorts All treated patients 22 1 95% Subtherapeutic ≤2 cycles 10 0 100% Therapeutic 3 cycles and phase 3-eligiblea 10 1 90% BCVA change from baseline(ETDRS letter score) Median change in BCVA in phase 3-eligible participants with therapeutic regimen (N=10)a Visual acuity was preserved in 90% of phase 3-eligible patients receiving a bel-sar therapeutic regimen 80% were at high risk of vision loss with tumors < 3 mm to the fovea or optic nerve 90% visual acuity preservation supports the potential forbel-sar to be a front-line therapy for early-stage disease aOne participant with circumpapillary tumor that did not meet phase 3 criteria is not included. bVision acuity loss defined as ≥15 letters decrease from baseline in ETDRS BCVA letter score. BCVA, best-corrected visual acuity; ETDRS, Early Treatment Diabetic Retinopathy Study. ClinicalTrials.gov Identifier, NCT04417530: AU-011-202. Data on file, Aura Biosciences. Study week (relative to first dose in Cycle 1) Vision preservation in9/10 participants Loss of 18 letters in one patient with progression of preexisting juxtafoveal fluid under fovea -5 0 5 -5 -10 -15 0 13 26 39 52

Bel-sar treatmenthad a favorablesafety profile No posterior inflammation No treatment-related SAEs No grade 3–5 treatment-related AEs * Table presents participants with AEs related to bel-sar or laser by severity and overall; participants with >1 AE are counted in the highest severity group AE, adverse event; SAE, serious adverse event; IQR, interquartile rangeClinicalTrials.gov Identifier: NCT04417530; AU-011-202. Data on file, Aura Biosciences. All treated participants (n=22)* Drug/laser-relatedadverse events Grade I Grade II Grade III-V Total Anterior chamber inflammation** 4 (18.2%) 0 0 4 (18.2%) Anterior chamber cell** 2 (9.1%) 0 0 2 (9.1%) Eye pain 2 (9.1%) 0 0 2 (9.1%) Anisocoria 1 (4.5%) 0 0 1 (4.5%) Conjunctival edema 1 (4.5%) 0 0 1 (4.5%) Cystoid macular edema 1 (4.5%) 0 0 1 (4.5%) Pupillary reflex impaired 1 (4.5%) 0 0 1 (4.5%) Salivary gland enlargement 0 1 (4.5%) 0 1 (4.5%) **Median duration 6 days (IQR: 3–10 days); All resolved with no or minimal treatment; If topical steroids given, median treatment duration 6 days Phase 2 safety outcomes (bel-sar/laser-related)

ClinicalTrials.gov Identifier: NCT06007690; AU-011-301. Phase 2 data support phase 3 assumptions Phase 3 trial design P < 0.005 93% power (Δ20) Actual data (Δ60) >99% power P < 0.05 Robustness analysis of tumor control rates Overall ratein phase 2 2x “worse” than phase 2 2x “worse” than phase 2 Actual ratewith documented growth inphase 2 Overall ratein phase 2 94% power (Δ30) Actual data (Δ60) >99% power Same dose, regimen, route of administration, range of tumor sizes, and reading center as phase 2 trial Similar population to phase 2 participants receiving the therapeutic regimen Enriching for early documented growth; phase 3 randomization stratified by growth rate

Appendix Urologic Oncology

aBCG failure in patient C3 qualifying as high risk by AUA criteria. AUA, American Urological Association.Clinicaltrials.gov identifier: NCT05483868; AU-011-102. Patient population: AUA risk classification and grade at screening Low-grade High-grade Low-risk Intermediate-risk High-risk Drug only: Patient 3 Drug only: Patient 4 Drug + light: Patient A3 Drug + light: Patient B2 Drug + light: Patient B3 Drug + light: Patient A2 Drug + light: Patient A4 Drug + light: Patient B1 Drug only: Patient 1 Drug only: Patient 2 Drug only : Patient 5 Drug + Light: Patient A1 Drug + light: Patient C1 Drug + light: Patient C3a Drug + light: Patient C2

Bel-sar, belzupacap sarotalocan; NMIBC, non-muscle-invasive bladder cancer; TURBT, transurethral resection of bladder tumor.Clinicaltrials.gov identifier: NCT05483868; AU-011-102. Phase 1 trial of bel-sar for bladder cancer designed to evaluate safety, feasibility, and mechanism of action Safety Review Board completed after each cohort. Patients followed for safety after TURBT to 56 days. Total 100 µg NMIBC (N=4) 50 µg at tumor base 50 µg within lamina propria Cohort A: Drug + light Total 100 µg NMIBC (N=3) 100 µg at tumor base Cohort B: Drug + light Study objectives Safety & dose-limiting toxicity Focal distributionof bel-sar Feasibility of technique Focalnecrosis Markers ofimmune activation Histopathological assessment completed at time of standard of care TURBT Part 1 (n=5) bel-sar + focal light activation Single dose window of opportunity study in NMIBC all-comers bel-sar alone Part 2 (n=~10) Cohort C: Drug + light Total 200 µg NMIBC (N=3) 200 µg at tumor base Total 100 µg NMIBC (N=5) 50 µg at tumor base 50 µg within lamina propria Drug only (No light)
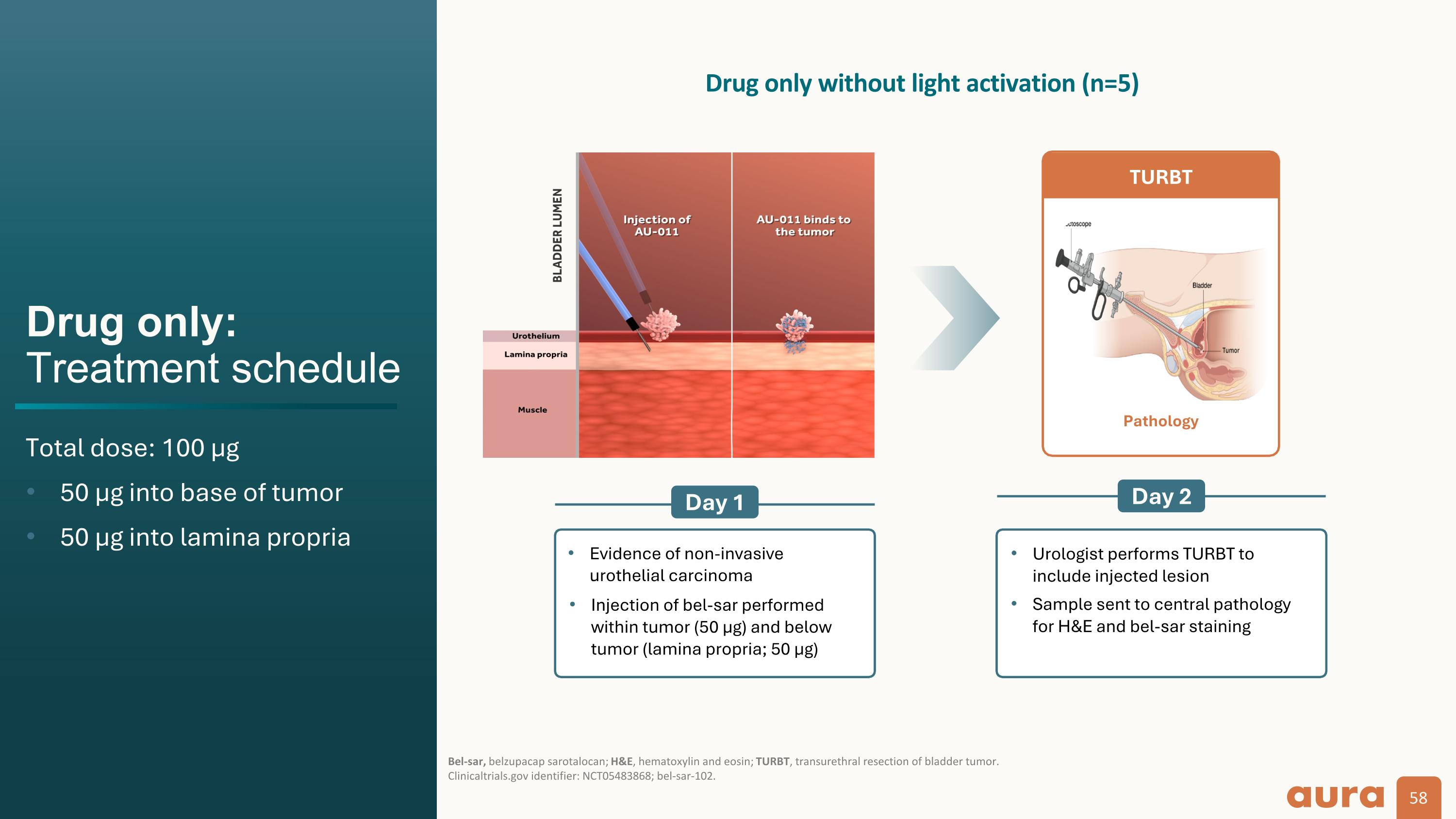
Drug only:Treatment schedule Total dose: 100 µg 50 µg into base of tumor 50 µg into lamina propria Bel-sar, belzupacap sarotalocan; H&E, hematoxylin and eosin; TURBT, transurethral resection of bladder tumor.Clinicaltrials.gov identifier: NCT05483868; bel-sar-102. Drug only without light activation (n=5) Day 1 Day 2 Evidence of non-invasive urothelial carcinoma Injection of bel-sar performed within tumor (50 µg) and below tumor (lamina propria; 50 µg) Urologist performs TURBT to include injected lesion Sample sent to central pathology for H&E and bel-sar staining Pathology TURBT
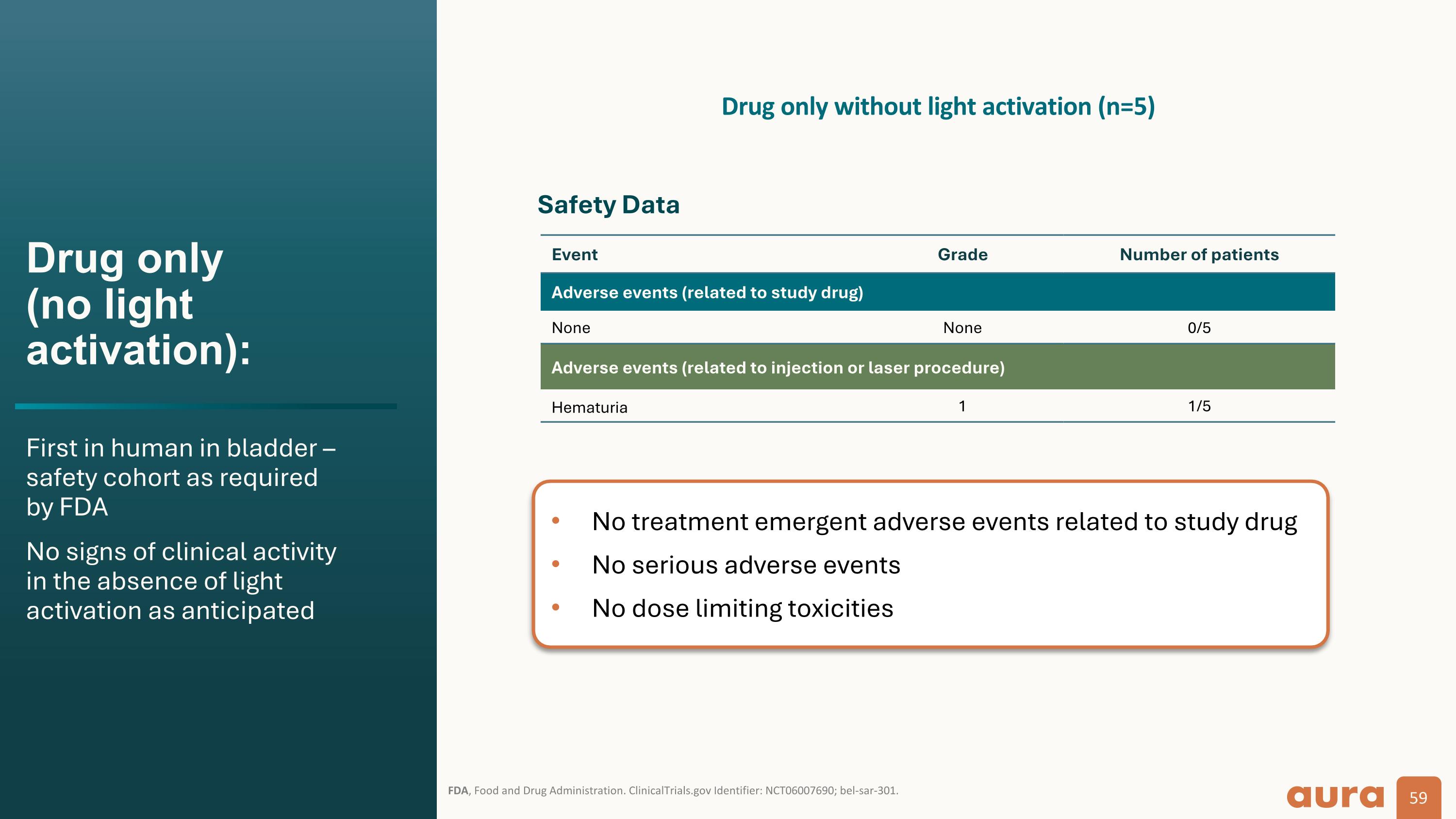
Drug only (no light activation): First in human in bladder – safety cohort as required by FDA No signs of clinical activity in the absence of light activation as anticipated FDA, Food and Drug Administration. ClinicalTrials.gov Identifier: NCT06007690; bel-sar-301. Drug only without light activation (n=5) Event Grade Number of patients Adverse events (related to study drug) None None 0/5 Adverse events (related to injection or laser procedure) Hematuria 1 1/5 Safety Data No treatment emergent adverse events related to study drug No serious adverse events No dose limiting toxicities